How data platforms help healthcare organizations leverage their massive data asset
Hospitals produce a staggering average of 50 petabytes of data each year, or 137 terabytes per day, every day. And shockingly, as much as 97% of that data goes unused. Today, approximately 30% of the world's data volume is being generated by the healthcare industry. By 2025, the compound annual growth rate of data for healthcare will reach 36%.
HIMSS and Arcadia partnered to conduct a survey of healthcare leaders to understand how they use data today and intend to use it in the future. Jake Hochberg, VP of Analytics and Chief Analytics Officer at Arcadia and Eric Gallagher, CEO of Ochsner Health Network offered their insights from that research in the webinar, The State of Healthcare Analytics.
Healthcare data platforms act as a single source of truth
Data platforms act as a single source of truth. Hochberg and Gallagher both agree there is high value in having a central location for data.
“The more you can have your data in one place, the more you can stitch the various components together, the less time you have to spend trying to grab data from system x and clean it so that you can compare it to system y and tell a story,” said Hochberg.
For example, in a value-based care platform, when claims data and referral optimization data are in the same place, organizations can leverage those two data sources together to build out preferred provider networks, and evaluate their ability to steer care towards those preferred provider networks without crossing multiple systems.
Gallagher notes that to be successful you have to educate a much broader audience of stakeholders on the business of medicine with a value-based care lens. And you have to democratize the data and analytics for the whole care delivery system.
“I see having that data platform as a huge enabler to get us all to be speaking the same language, which is sort of a new language for a lot of people,” he said.
Multiple barriers to investing in healthcare data platforms

In the HIMSS/Arcadia survey, 70% of healthcare organizations said other strategic priorities get in the way of investing in analytics. Other reasons organizations said they put investments in analytics on the backburner were limited staff resources, staff resourcing training, lack of budget, inability to integrate existing workflows, organizational resistance, and security concerns.
Unfortunately, this attitude is short-sighted. As Hochberg said, “If you're in a value-based agreement, often you are competing against some form of a national trend to regional trend. Even in fee-for-service, you're to an extent competing for patient volume, you're competing for negotiating power, so there's an element of almost not having a choice. If you want to be able to keep up in healthcare, you're going to need to invest in analytics.”
He believes we've moved to a point where it's less of a question of should we use data and it's more of a question of do we have the right resources to use data and that organizations are trying to optimize the strategy of rollout versus deciding if they should purchase a system.
Gallagher added his insight another motivator for data platforms: the healthcare labor shortage.
“A number of surveys talk about the healthcare labor shortage as the single biggest challenge in the healthcare industry today and so when you think about the workforce, and how to prioritize investments in data and analytics and digital tools and automation, think about it from the workforce perspective,” he said.
These tools and insights empower your workforce, which drives engagement and retention. In turn, an engaged, empowered, and satisfied healthcare workforce yields an engaged and empowered, and satisfied patient population.
“There's the financial reimbursement movement — that's a big part of the equation — but you can make it about your workforce as well and there's no bigger priority than that right now,” added Gallagher.
Enabling a paradigm shift with healthcare data

Traditionally, healthcare organizations are somewhat risk averse and this new reality is no different. Healthcare organizations aren’t jumping on board with lightning speed. They said on average, only 57% of their data is being used to make decisions. In addition, 29% of IT tech and clinician roles report resistance from executive leadership with adopting new solutions (executives at smaller organizations are even more resistant.)
“Part of the vision and communication is really this paradigm shift that's going to be required,” said Gallagher.
He advises organizations to talk about the risk of not changing and not improving as being greater than those risks that come with the change.
“You don't want to become the Blockbuster in a world of Netflix's, Amazons, and Apples,” he said.
Hochberg added that another reason for resistance is that organizations have systems they've built and finely tuned for their organization for some hyper-specific use cases.
“The smaller you are and the closer you are to those systems, it can be hard to move away to a larger data platform, or you might be able to get more scale and create more analytics and answer more use cases and questions, but you're going to trade off a little bit of that very precise data accuracy,” he explained.
Adoption across organizations is also challenging. In the survey, 40% of healthcare organizations reported that clinicians and analysts resist adopting new solutions and 42% reported challenges with integrating the tools that they're rolling out with existing workflows. It can be hard to pivot, which is why top-down alignment is critical. To achieve adoption, Hochberg recommends starting at the executive level to ensure everyone buys in and agrees to try.
“Additionally, sometimes when you switch some type of platform that you're going to actually experience inefficiency before you gain efficiency and accepting that, planning for it, and buying into that is another really important piece,” he points out.
Gallagher says alignment around incentives helps as well.
“You have to connect the dots between using this tool, using these data and analytics to the desired outcome and why that desired outcome is beneficial for the patient, or doing this extra piece of work is also beneficial to the organization,” he explained. “But if it's beneficial to the organization and not the provider, then that's problematic as well, so cascading from the incentives to the organization to the provider to the patient is really important.”
Will AI change the way we will deliver healthcare?
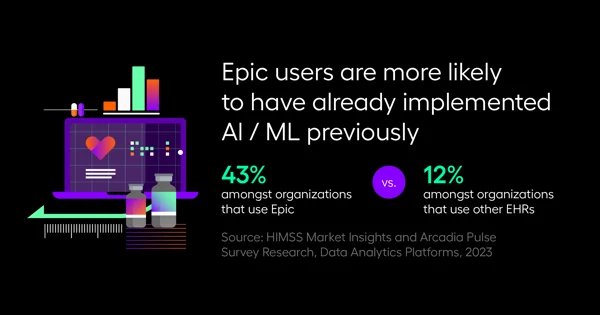
In the survey, AI and machine learning was reported to be the least implemented technology today, though it was the highest priority within the next two years.
“We do tend to over expect from new data and tech innovations in the short term and under expect from them in the future. So I think from a workflow, direct patient outcomes perspective, it'll still be a little while before AI is fully baked into the systems and I think there's always going to need to be a human element,” said Hochberg.
He says AI in the short term is going to have more of an impact on productivity of individuals—the ability to take notes faster, the ability to write patient emails faster—before it actually changes or automates decision making for a patient.
Gallagher says at Ochsner, he’s prioritizing AI to make the best use of limited resources and make smaller, meaningful improvements.
“I know that I don't have enough care coordinators, case managers, or IDI, navigators, community health workers, for the number of patients that we are accountable for, so I'm prioritizing AI to make the best use of those limited resources that we have for the most vulnerable and impactful patients with the right interventions or the right support at the right place at the right time,” he said.
To learn more about ways Arcadia can advance your data analytics capabilities to meet the future of healthcare today, talk to an Arcadia representative or watch the webinar replay.



