
HEALTHCARE DATA PLATFORM
Curated insights.
Top payers and healthcare providers trust Arcadia to deliver insights where they matter most.
We’re proud to partner with healthcare innovators:














Higher savings
Arcadia customers earned $126 PMPY more savings than non-Arcadia customers
Increase in BCDA lives
Processed in 9 months across customers
Higher MSSP bonuses
Arcadia customers have achieved higher MSSP bonuses through improved care coordination and higher quality measures
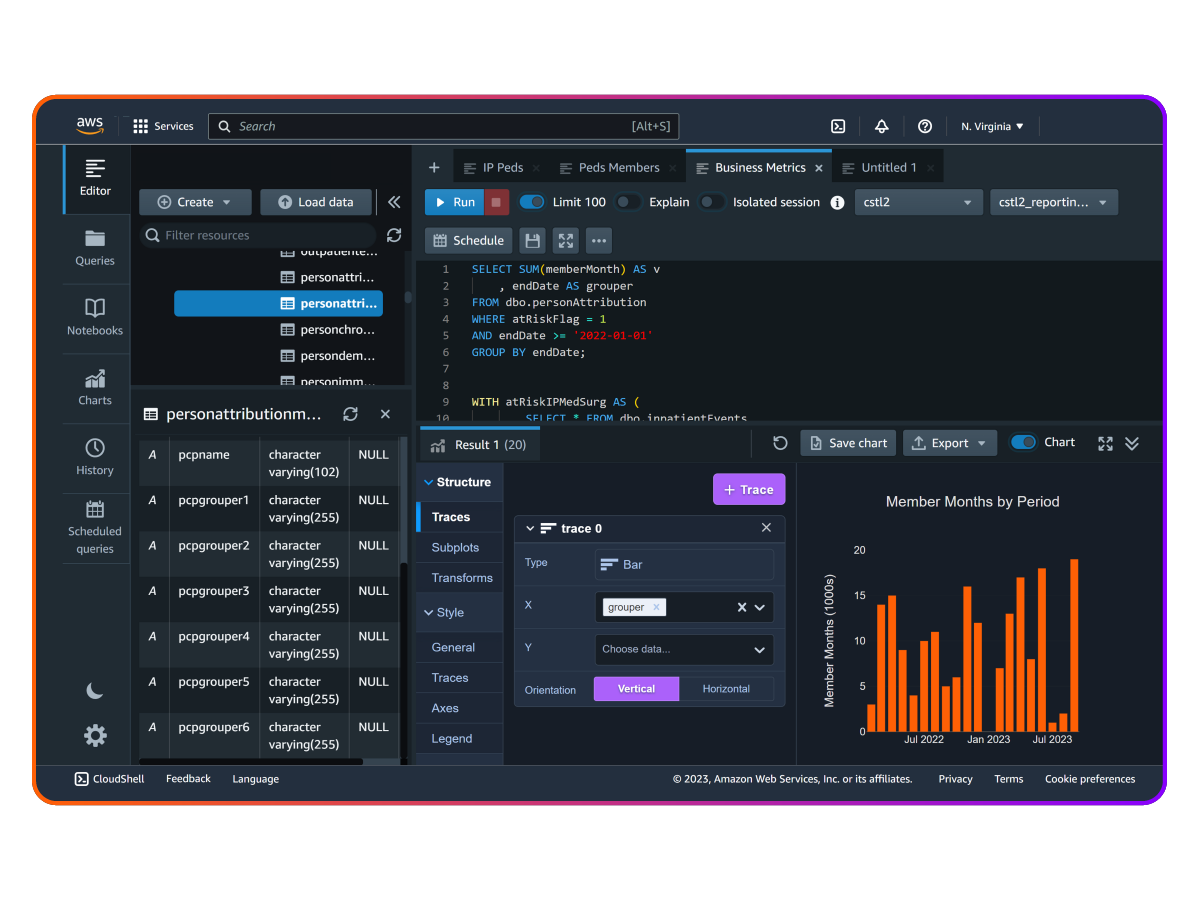
Aggregate
Build a unified data foundation
Amass disparate healthcare data into a flexible platform, unifying EHRs, claims, SDoH information, and other critical sources. With comprehensive data aggregation, Arcadia creates a foundation for impactful analytics and AI.
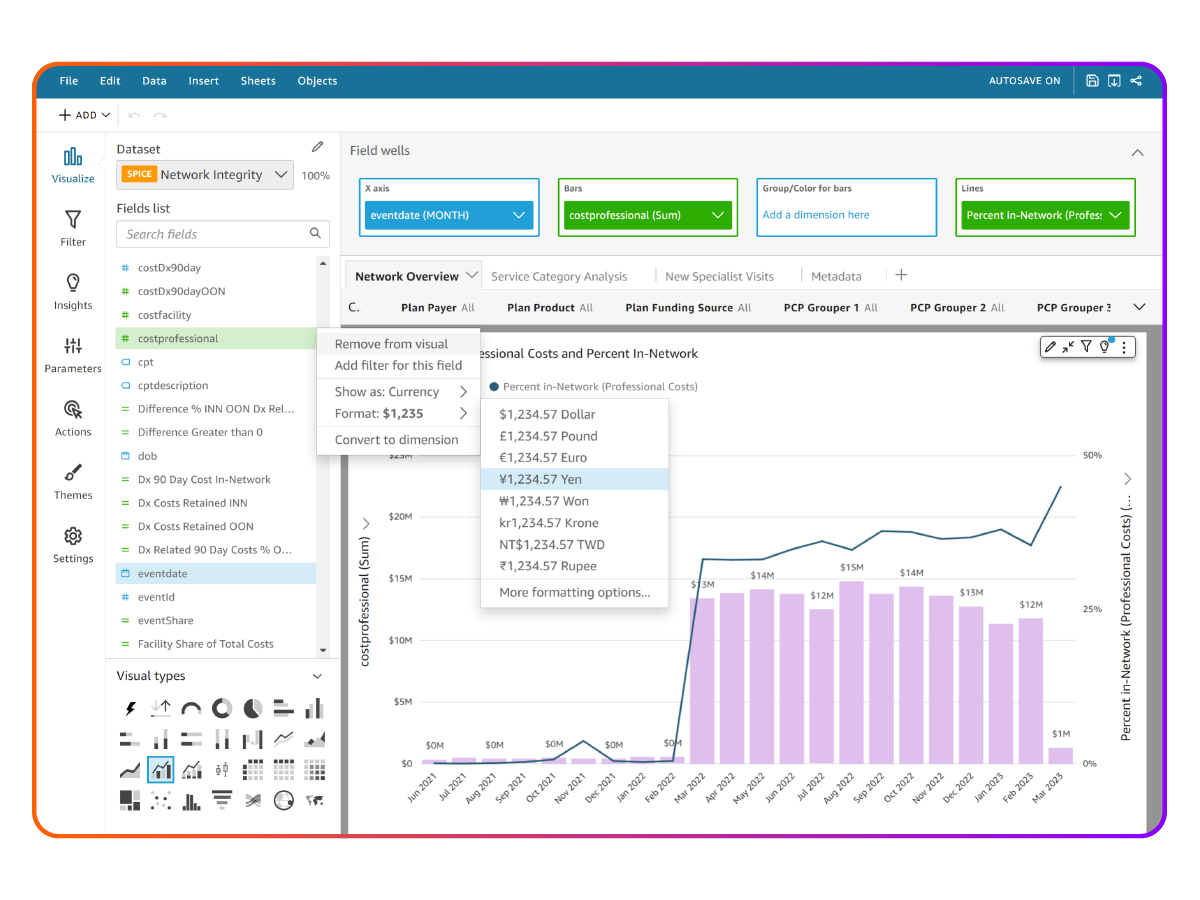
Analyze
Extract meaningful insights
Cut through the noise to uncover actionable insights. Arcadia’s analytics software enables healthcare teams — from analysts to clinicians to strategic decision-makers — to identify key patient populations, assess risk, and drive interventions.
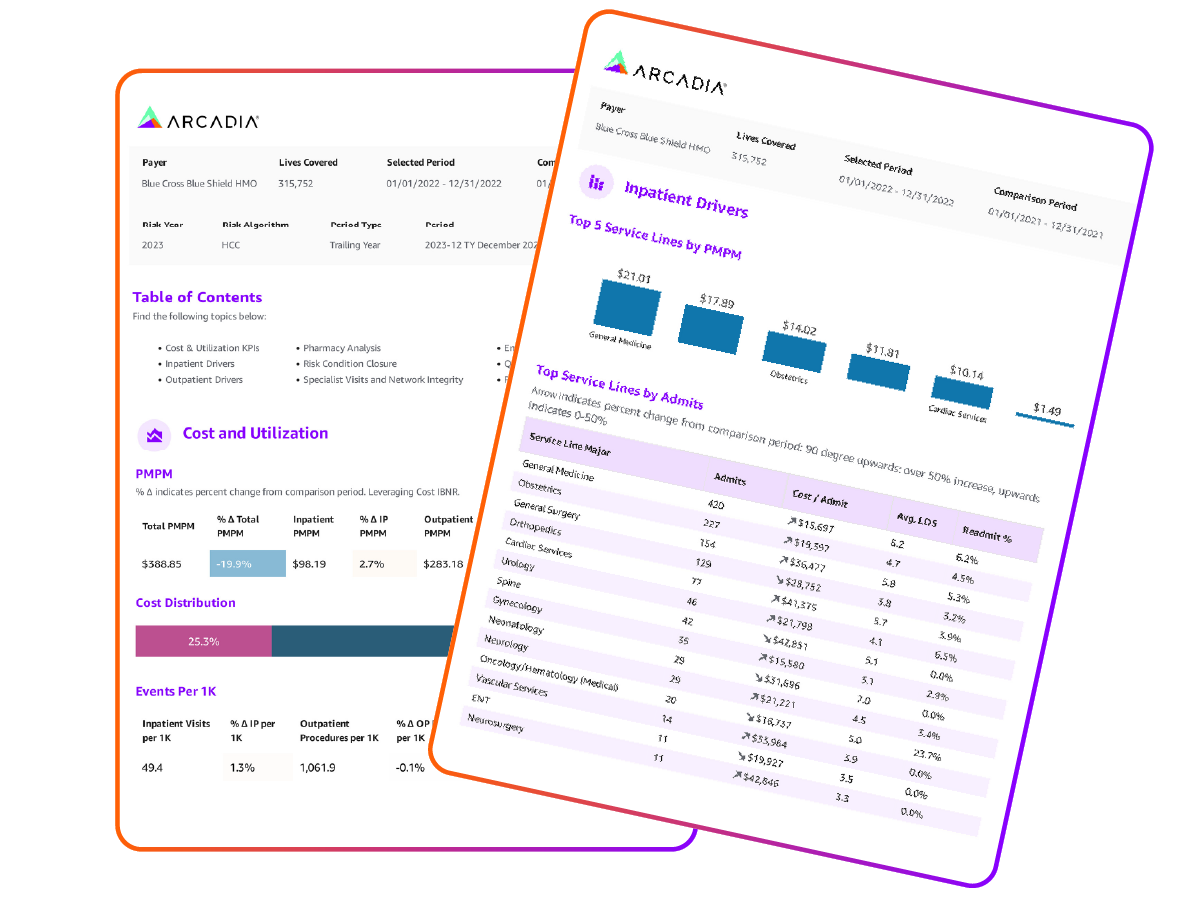
Activate
Transform insights into action
Empower teams with tiered access, delivering the information your users need when and where they need it. From interoperable applications at the point of care to dashboards and PHI-free documents, Arcadia delivers intelligence that drives better care, increases revenue, and reduces costs.
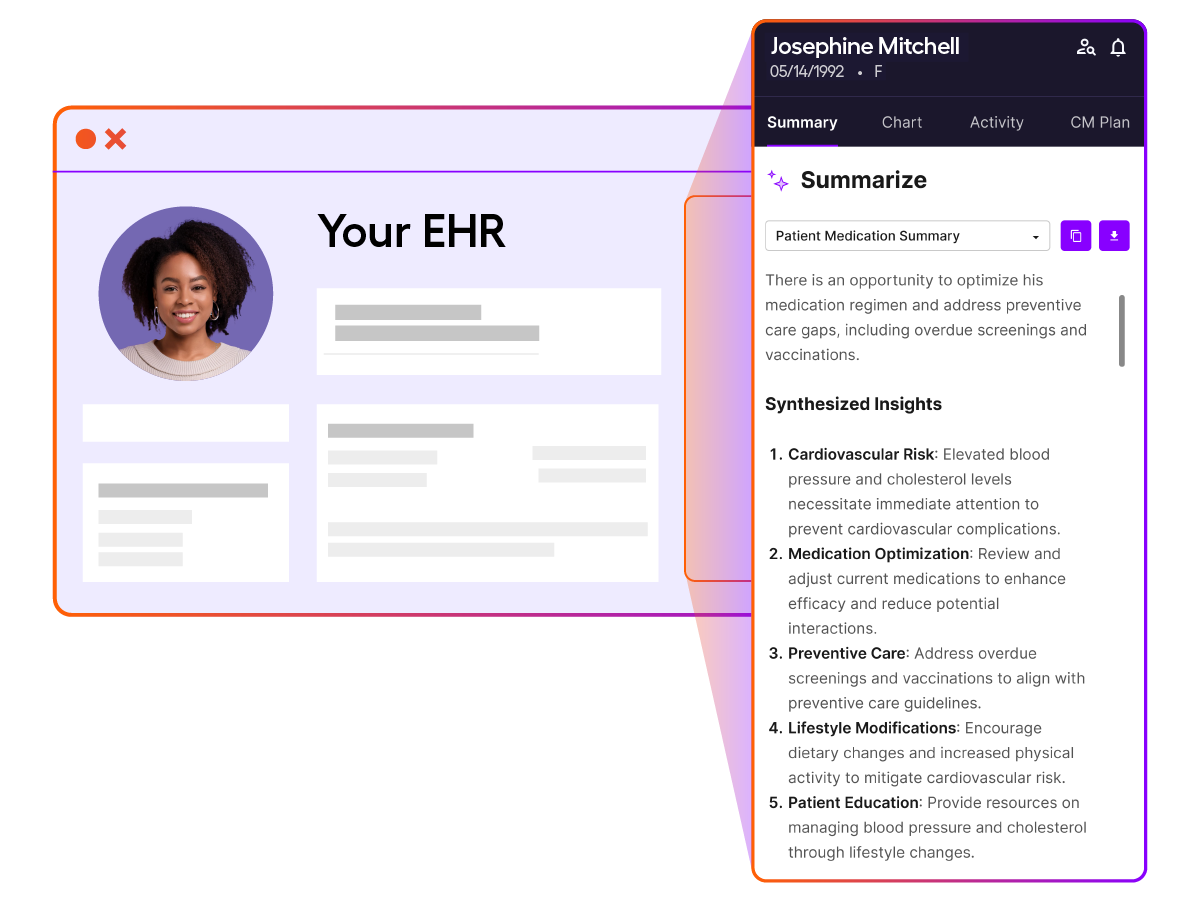
Automate
Improve efficiency and impact
Put data to work by streamlining workflows and automating routine processes, freeing up your teams to focus on what matters most. Arcadia’s AI and machine learning capabilities drive faster, more effective healthcare operations to boost clinical and financial success.
Healthcare analytics software designed for transformation


All your data, one platform
Unify disparate sources and power AI models, reports, and dashboards — all from a single source of truth.

Analytics that drive action
Out-of-the-box insights on a scalable platform built for healthcare to empower every team in your organization.

Your ally in innovation
With deep expertise in value-based care, healthcare, data, and analytics, Arcadia is dedicated to achieving financially sustainable healthcare.

Healthcare’s insight hub
Arcadia is healthcare’s market-leading data platform, with a connected ecosystem of integrations and partners to drive results across the care continuum.

Fueling innovation for healthcare’s top performers
Arcadia partners with industry leaders who are shaping the future of care delivery. Proudly serving over 30% of Newsweek’s 2024 Best Hospitals and top performers in MSSP and ACO REACH, Arcadia clients deliver measurable value to their bottom line drive via comprehensive healthcare analytics.
Advanced analytics for every corner of healthcare

Payers
Gain insights into member populations, manage risk, and track quality metrics, enabling better decision-making for value-based care and cost savings.

Health Systems
Integrate disparate data sources, improve care coordination, and enhance patient outcomes by providing clinicians with a comprehensive view of patient health.

Accountable Care Organizations (ACOs)
Track performance metrics, optimize care management, and maximize savings through advanced data analytics and population health insights.

Government
Support public health initiatives, streamline data integration, and monitor population health, facilitating informed policy-making and program effectiveness.
Accelerate your path to exceptional results
Find out how you can deliver actionable insights to your teams, optimize operations, improve patient and member outcomes, grow your network, and support value-based initiatives — all on a data platform that drives meaningful results for healthcare’s leading organizations.





 >
>