CMS’ 10-Year Bet on Accountable Care: Understanding LEAD
Editor’s note: This is the first in a series on CMS’ new LEAD model. Future posts will explore benchmark methodology, population segmenting, and risk scoring.
On March 31st, 2026, CMS released details on a new model called LEAD — the Long-term Enhanced ACO Design. It’s positioned as a replacement for ACO REACH. However, LEAD is not just an evolution of ACO REACH. It’s a fundamentally different proposition: a ten-year model with a fixed benchmark that never rebases, an integrated approach to high-needs populations, a ramp designed to bring in organizations that have never participated in value-based care, and a plan to eventually replace traditional risk adjustment with artificial intelligence.
This article explains what the model is, why it is structured the way it is, and why CMS designed it to attract providers who have historically stayed on the sidelines.
The LEAD Model Pitch: Ten Years, No Rebasing
The single most important design feature of LEAD is its benchmark structure. Benchmarks in MSSP get recalculated every agreement period. Organizations that do a good job of managing costs receive a lower benchmark (higher performance threshold) the next time around. ACOs have complained about this for years because it creates a dynamic where success is punished and savings today become targets tomorrow.
LEAD eliminates this entirely. The benchmark baseline is set using three calendar years of spending data (CY2024, CY2025, and CY2026), and that baseline is fixed for the entire ten-year model. It’s trended forward each year using a blend of national growth rates, regional growth rates, and the Accountable Care Prospective Trend (ACPT), which is an upfront projected growth factor, not an observed national or regional trend. However, the underlying historical spending is never recalculated.
The implications are significant. An ACO that enters LEAD in 2027 and consistently reduces costs over time will see the gap between its benchmark and its actual spending widen year after year. CMS calls this the "savings wedge." It is the structural opposite of the rebasing cycle in MSSP.
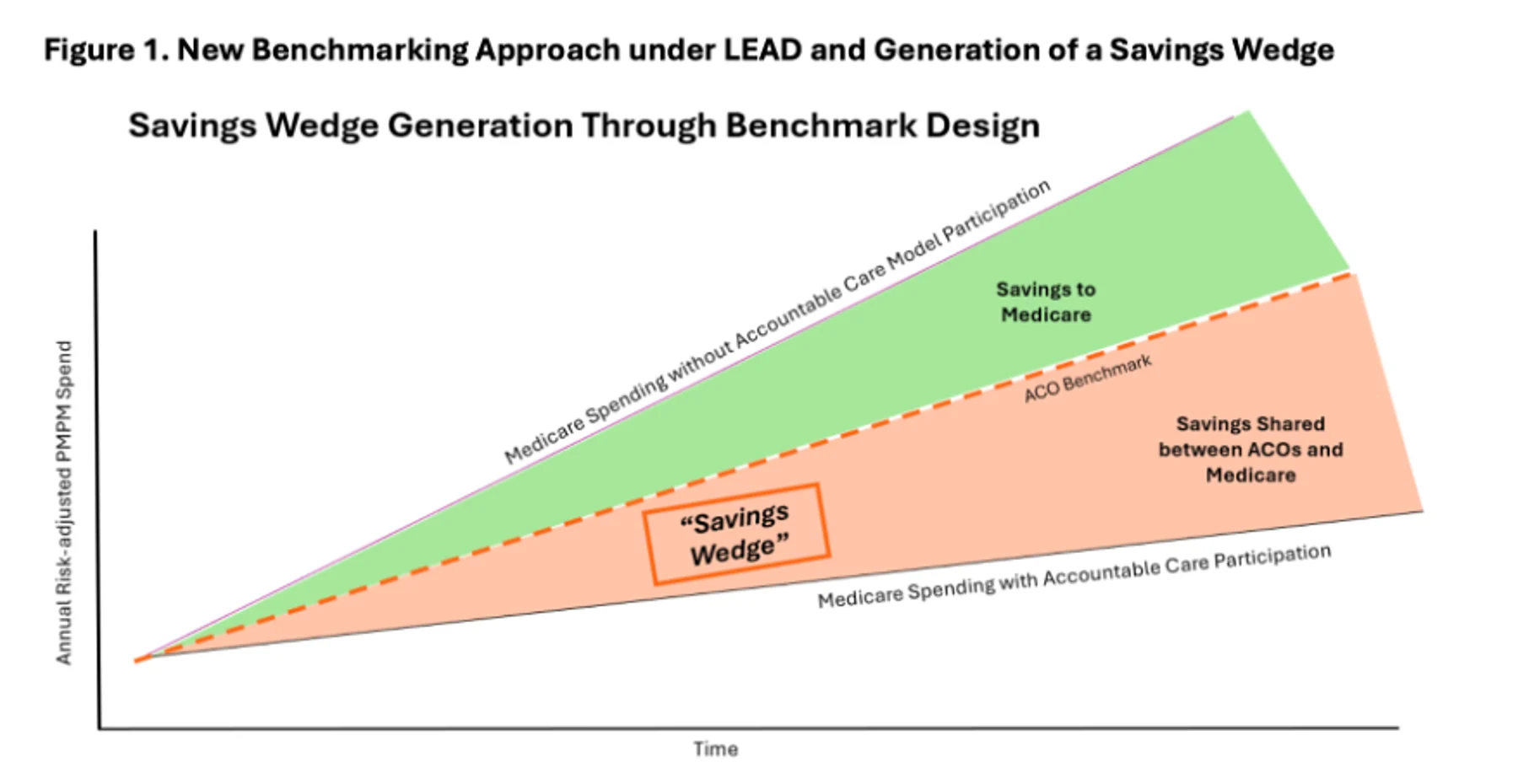
Whether it works as intended over a decade is uncertain. CMS has never tried anything similar at this scale. However, the theory is sound, and the incentive alignment is clear: get better, keep more. CMS has listened to ACOs' suggestions over the last few years and responded with a benchmarking strategy designed to alleviate their concerns.
A reasonable question on this strategy: what happens when healthcare costs change dramatically over ten years due to factors no one anticipated? CMS has built in guardrails in the form of caps on the ACPT component of the benchmark, but the honest answer is that we’ll find out. Ten years is a long time. A lot can happen. The last decade taught us that much.
Who LEAD Is Really For
The obvious targets for LEAD are organizations already in ACO REACH. These organizations have the infrastructure, the contracts, the experience with risk, and a model that ends on December 31, 2026. The transition path is straightforward. CMS has even made the application process simpler for existing REACH ACOs.
But LEAD's design suggests CMS is after a much larger audience. Several features of the model only make sense if viewed as deliberate on-ramps for organizations that have never participated in a total-cost-of-care model before. Other features, such as total risk and many of the available beneficiary enhancements, are enticing to groups that have historically operated in Medicare Advantage. Many MSSP ACOs have asked for total cost of care risk tracks. The similarities in benchmark calculation, especially with the ACPT, look a lot like the total cost of care risk corridor MSSP ACOs are asking for.
Rural and Small Providers
LEAD allows newly entering ACOs to start with as few as 1,000 aligned beneficiaries and ramp to the standard 5,000 minimum over five years. For context, MSSP requires 5,000 from day one. A rural health system with a modest Medicare FFS panel that could never hit MSSP's threshold on enrollment day can now enter LEAD and build its population over time.
The model also allows mid-year TIN additions under a "hybrid" alignment option — meaning an ACO can bring new provider groups into its network during the performance year, not just at the start. For smaller organizations still building provider networks, this flexibility is meaningful. Those organizations need not have everything perfectly assembled before the starting gun fires.
There is also a 1.5% administrative add-on for higher-spending ACOs. This is a capitated payment: upfront money that is explicitly not included in the reconciliation calculation and not subject to repayment. It’s designed as startup capital for organizations that spend more than their regional average and need investment to build the care management infrastructure required to bring those costs down. To entice participants who have been sitting on the sidelines due to the administrative costs of participating in value-based care models, CMS acknowledges that infrastructure costs money before it saves money, and they’re willing to fund that ramp.
Providers Serving High-Needs Populations
In ACO REACH, "high needs" was a separate ACO track. LEAD integrates high-needs concepts across ACOs. Any beneficiary meeting certain clinical criteria (mobility impairment, frailty, high risk scores, frequent hospitalizations, extended SNF stays, etc.) is designated high needs, and that designation is permanent for the life of the model. These beneficiaries receive a separate benchmark and a separate concurrent-year risk-adjustment model to predict costs.
Why does this matter? Because the standard prospective HCC model—the one most organizations are used to—predicts next year's costs based on last year's diagnoses. For a complex patient whose condition deteriorates rapidly, that model systematically underpredicts. A patient who had a stroke in March will generate diagnoses that do not appear in the risk model until the following calendar year. In the meantime, the ACO is responsible for costs that its benchmark was not built to absorb. The concurrent model addresses this by using real-time diagnostic information for patients deemed “high needs.” For organizations that serve large numbers of medically complex patients, including PACE-like programs, safety-net systems, and organizations with significant dual-eligible populations, this is a structural improvement in how their population's costs are recognized and funded.
ACOs where at least 40% of aligned beneficiaries are high needs also qualify for a lower alignment minimum, starting at 800 instead of 5,000. This is an explicit invitation to PACE organizations, high-needs-focused provider groups, and others serving populations that prior models struggled to accommodate.
The "Non-VBC" Provider
There is a category of provider organization that has watched MSSP and ACO REACH from the sidelines. They’re aware of value-based care, possibly interested, but never quite convinced the math worked for them. Maybe they are in a high-cost market and worried about an unfavorable benchmark. Maybe they are physician-led and lack the administrative infrastructure. Maybe they looked at MSSP's two-sided risk tracks and decided the downside exposure was not worth the potential upside.
LEAD's professional risk option limits downside to 50% of losses, with risk corridors that further reduce exposure at higher loss levels. The first corridor absorbs losses up to 10% of the benchmark at a 50% share rate. By the time losses exceed 20% of the benchmark, the ACO's share drops to 5%.
This is not risk-free. It’s real two-sided risk. But the corridor structure means that even a bad year does not produce a catastrophic financial outcome. Combined with the no-rebasing guarantee and the first-dollar savings structure (no minimum savings rate before earnings), the model is designed to make the risk calculus work for organizations that previously concluded it did not.
What Comes Next for the CMS LEAD Model
Applications for LEAD open May 17. The first performance year begins January 1, 2027.

