Identifying the right patients at the right time
Maximizing effective care management with Arcadia Impact Suite
One of the most significant challenges healthcare providers face is identifying the right patients for care management programs. With the ever-growing demands on care teams and the ongoing shortage of nursing and medical staff, it is crucial to find efficient and effective ways to provide quality care to patient populations.
In this article, we will explore how data management and advanced algorithms, such as Arcadia’s Impact Suite, can revolutionize the process of identifying impactful patients, streamlining care management, and ultimately improving patient outcomes. We also addressed this topic in a Byte-Size Booth talk at HIMSS, which features Carissa Crawford, Sales Director at Arcadia.
Challenges in traditional data management approaches

In this Byte-Size Booth Talk, Carissa Crawford sheds light on the limitations of traditional patient identification approaches. Crawford states, “We see a really common theme of looking at the highest cost members or who is starting to become a higher cost or rising risk. The idea is we get ahead of some increased uptick in costs and start to get those patients back on a well-managed, well-cared-for trajectory that they might have once been on.”
While this approach may have served its purpose in the past, it did not necessarily address the concept of impactability — the potential positive impact of interventions on patient outcomes and cost management. Using risk-adjustment algorithms for stratification purposes can lead to less accurate patient identification and missed opportunities for effective care management.
Crawford further emphasizes the challenges faced by care teams. She states, “Care programs often include the entire care team, from physicians to social workers to pharmacists to nurses, who are all trying to be asked to do more with less time.”
Impactability: Leveraging patient data for effective care management
Arcadia’s Impact Suite, which includes algorithms such as the CCM Impact Score, takes a revolutionary approach to care management by introducing the concept of impactability. Crawford explains, “We believe that data does exist. We’ve developed a suite of algorithms that help us tell that story and narrative around impactability.”
By analyzing patient data from over 170 million patient records, these algorithms can determine the delta between a patient’s care outcome and the cost of managing them. This data-driven approach enables care teams to quantify the true impact of interventions, resulting in more effective patient care.
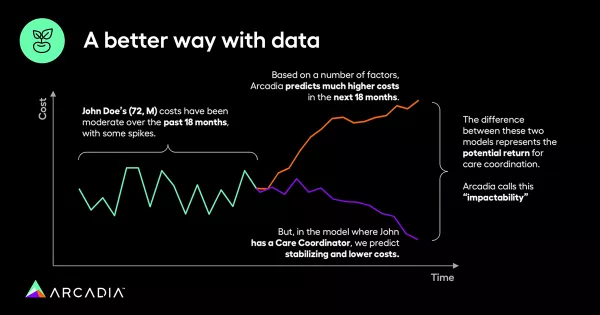
“We start to see a quantifiable difference in the utilization pattern, the cost of John Doe’s care as well as the quality of life that he’s living in the care outcomes of that program,” Crawford illustrates, referring to the personalized patient data analysis that Arcadia’s Impact Suite provides. This analysis allows care teams to identify the optimal time to intervene with an appropriate care program, leading to quantifiable cost savings and improved patient well-being.
Data as the foundation of effective care management
“When it comes to maximizing the effectiveness of care management, it all starts with data,” Crawford states. For healthcare providers looking to implement data-driven approaches like Arcadia’s Impact Suite, the first step is to gather and analyze their own patient data.
Crawford emphasizes the significance of data integration and quality. “The first step for any customer is really to make sure that we’ve integrated the data and it’s of high quality and trustworthy. Without that, none of these interventions are really going to be as impactful as they can be.”
Identifying trends in clinical records and health plan data allows care teams to recognize areas of high impactability, such as behavioral health or transitional care. By forecasting and modeling potential outcomes of increased program utilization, care teams can make informed decisions on expanding care offerings.
A better way with data: Validating care interventions with the Arcadia Impact Suite
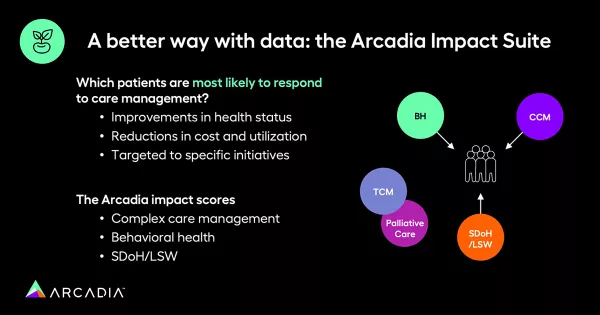
Another crucial aspect of effective care management is validating interventions’ success using data. Arcadia’s Impact Suite achieves this by comparing cohorts of patients who received care program enrollment with those who did not. By analyzing total costs, gap closure efforts, and overall care quality, care teams can measure the true impact of their interventions.
“By analyzing the data, you can start to run some of these algorithms and see what percentage of your population falls into a category we would consider highly impactful or strongly impacted,” Crawford explains. This data-driven validation allows care providers to continually fine-tune their care management strategies, ensuring the best possible outcomes for their patients.
As healthcare providers, we face numerous challenges in delivering effective care management, especially in the face of staffing shortages and rising patient panel sizes. However, by harnessing the power of patient data and advanced algorithms like Arcadia’s Impact Suite, we can identify the right patients at the right time, maximize the impact of our care programs, and improve patient outcomes significantly.
Crawford’s insights further highlight the importance of data-driven decision-making in modern healthcare. By starting with data and integrating it seamlessly into our care management processes, we can make data-driven decisions that result in more efficient, cost-effective, and patient-centric care. Embracing these technological advancements and prioritizing data management will undoubtedly shape the future of healthcare, empowering us to provide the best possible care for our patients.
