KLAS Research: Arcadia’s care management solution scores highly for identifying and closing care gaps
Arcadia customers also laud platform’s data integration abilities across care settings to coordinate care2
Burlington, MASS. (Dec. 19, 2019) – Value-based care technology leader Arcadia (www.arcadia.io) announced today that highly-regarded third-party analyst KLAS Research recognized its population health management platform Arcadia Analytics for its ability to support identifying and closing gaps in care. Arcadia received a score of 8.7 out of 9 (limited data) for this capability.1 In their Population Health Care Management 2019 report, KLAS evaluated Arcadia’s care management capabilities versus its competitors and assessed the platform’s ability to support the work of care managers.
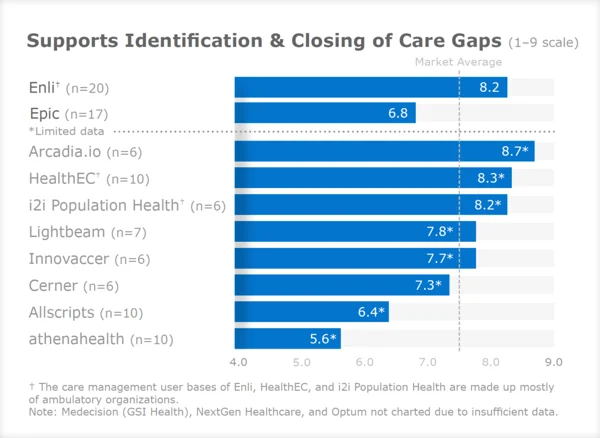
KLAS gave Arcadia Analytics its highest ranking of ‘above average’ for the platform’s ability to pull in data to create a longitudinal patient health record and then identify and close care gaps.3 “Arcadia’s software has a strong interface that allows integration into the physician workflow and their managed services experience has helped them develop tools that generate actionable insights around care gaps,” KLAS reported.2
Arcadia works with some of the largest and most advanced risk-bearing provider organizations in the country. Arcadia Medicare Shared Savings Program ACO customers performed 2.5 times better than non-customers in 2018, due in no small part to Arcadia’s ability to mine usable data from electronic health records (EHRs), marry that data with claims-based data from health plans, and get critical insights back into the existing workflows of physicians and care teams.
Arcadia Analytics uses this comprehensive population-level and patient-level data to help healthcare organizations easily identify and communicate care gaps to provider practices at the point of care. Pre-visit planning reports help care teams prepare to close care gaps during patient appointments. Providers can get a complete view of patient needs without leaving their EHR, thanks to an always-on desktop application that recognizes the patient record in the EHR and overlays associated care gaps from Arcadia Analytics — and all of this information is visible within care management workflows and reports as well.
“Being recognized by KLAS as a leader in care management solutions validates Arcadia’s approach to building population health management tools around a legacy of first-hand knowledge and understanding of provider needs to ensure guidance and success throughout the care management journey,” said Arcadia Executive Chairman, Board of Directors Sean Carroll. “Our focus has always been bringing together clinicians, data analysts, and administrators through a care management solution that acts as the glue in value-based performance programs, supporting high-quality care and improving the quality of life for patients.”
Arcadia customers highlighted the company’s ability to help care managers determine the clinical needs and health risks of each patient.
“The quality measures and additional data points that we pull through the platform are really helpful for our care managers in understanding patients’ condition histories. We can pull patients’ medication histories and clinical data. The data is clean. The data is shown in an easy way that enables us to see more information. It is nice to have a one-stop shop.”4
Predictive analytics: Finding patients most likely to benefit from care
KLAS researchers were particularly interested in how provider organizations “leverage data on social determinants of health (SDoH) (notoriously tricky to gather, manage, and make accessible) through their PHM system.”5 This has been a focus area for Arcadia as it aids customers in identifying the patients who are likely to benefit from care management. Arcadia defines success in care management as a reduction in emergency department visits, hospitalizations, readmissions, and a reduction in the total cost of care for patients who are under management versus an unmanaged control group.
Using predictive analytics, Arcadia helps providers identify patients who are most likely to benefit from intervention by a care manager. Because Arcadia’s algorithms assess health and socioeconomic markers in addition to traditional utilization metrics, Arcadia can surface patients from across a diverse population. Some patients meet more traditional criteria for care management, but others are “unexpected” candidates who have a history of low cost and/or low utilization but who have health and socioeconomic markers that suggest an opportunity to head off future adverse outcomes.
To learn more about how predictive analytics can support effective care management programs, please watch this talk from Arcadia chief medical officer Rich Parker, MD.
About KLAS
KLAS is a research and insights firm on a global mission to improve healthcare delivery. Working with thousands of healthcare professionals and clinicians, KLAS gathers data and insights on software, services and medical equipment to deliver timely, actionable reports and consulting services. KLAS represents the provider and payer voice and acts as a catalyst for improving vendor performance, highlighting healthcare industry challenges and opportunities, and helping build understanding and consensus for best practices. To learn more about KLAS, go to klasresearch.com.
About Arcadia
Arcadia is dedicated to happier, healthier days for all. We transform data into powerful insights that deliver results. Through our partnerships with the nation’s leading health systems, payers, and life science companies, we are growing a community of innovation to improve care, maximize value, and confront emerging challenges. For more information, visit arcadia.io.
# # #
References
- KLAS Research. Population Health Care Management 2019. Performance Report; December 2019: 3.
- KLAS Research. Population Health Care Management 2019. Performance Report; December 2019: 15.
- KLAS Research. Population Health Care Management 2019. Performance Report; December 2019: 15-16.
- KLAS Research. Population Health Care Management 2019. Performance Report; December 2019: 72.
- KLAS Research. Population Health Care Management 2019. Performance Report; December 2019: 9.
