Streamlined eCQM submissions with expert support
CMS’s standards change at breakneck speed — can you keep up? Without adequate data management, many ACOs are left scrambling to aggregate disparate data, transform it to the right format, and submit results at year’s end. Even if they are able to successfully submit, there are often unwelcome surprises, and all too frequently there are dollars left on the table.
There’s a better option. Arcadia’s ACO customers are leveraging our vast data analytics platform and partnership with ACO Health Solutions. Together, we provide a solution to collect, evaluate, package, and submit quality measures while offering mid-year insights into performance, so quality initiatives can be adjusted to maximize performance.
At the end of this year, submit with confidence, maximize returns, and crush your performance under MSSP and ACO REACH contracts.
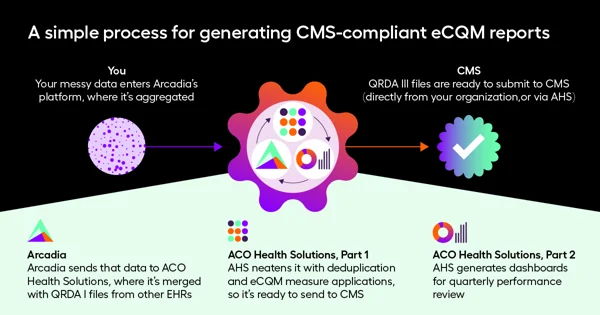
A simple process for generating CMS-compliant eCQM reports
- Your messy data enters Arcadia’s platform, where it’s aggregated
- Arcadia sends that data to ACO Health Solutions, where it’s merged with QRDA I files from other EHRs
- AHS neatens it with deduplication and eCQM measure applications, so it’s ready to send to CMS
- AHS generates dashboards for quarterly performance review
- QRDA III files are ready to submit to CMS (directly from your organization, or via AHS)
Qualified registry enabled 11 ACOs to submit eCQMs in 2022
Through this partnership, 11 ACOs have seen stellar results. The collaboration has resulted in:
- Timely insights into metrics and goals, enabling enhanced ability to tailor quality of care
- Easily meeting regulatory requirements (and qualifying for important savings and bonuses)
- Demonstrable, qualified value to patients and other stakeholders
Get a demo to see how you can aggregate your data in a format that adheres to eCQM standards on the Arcadia Analytics platform
