A lifetime of healthcare: The costs of 85 years of life
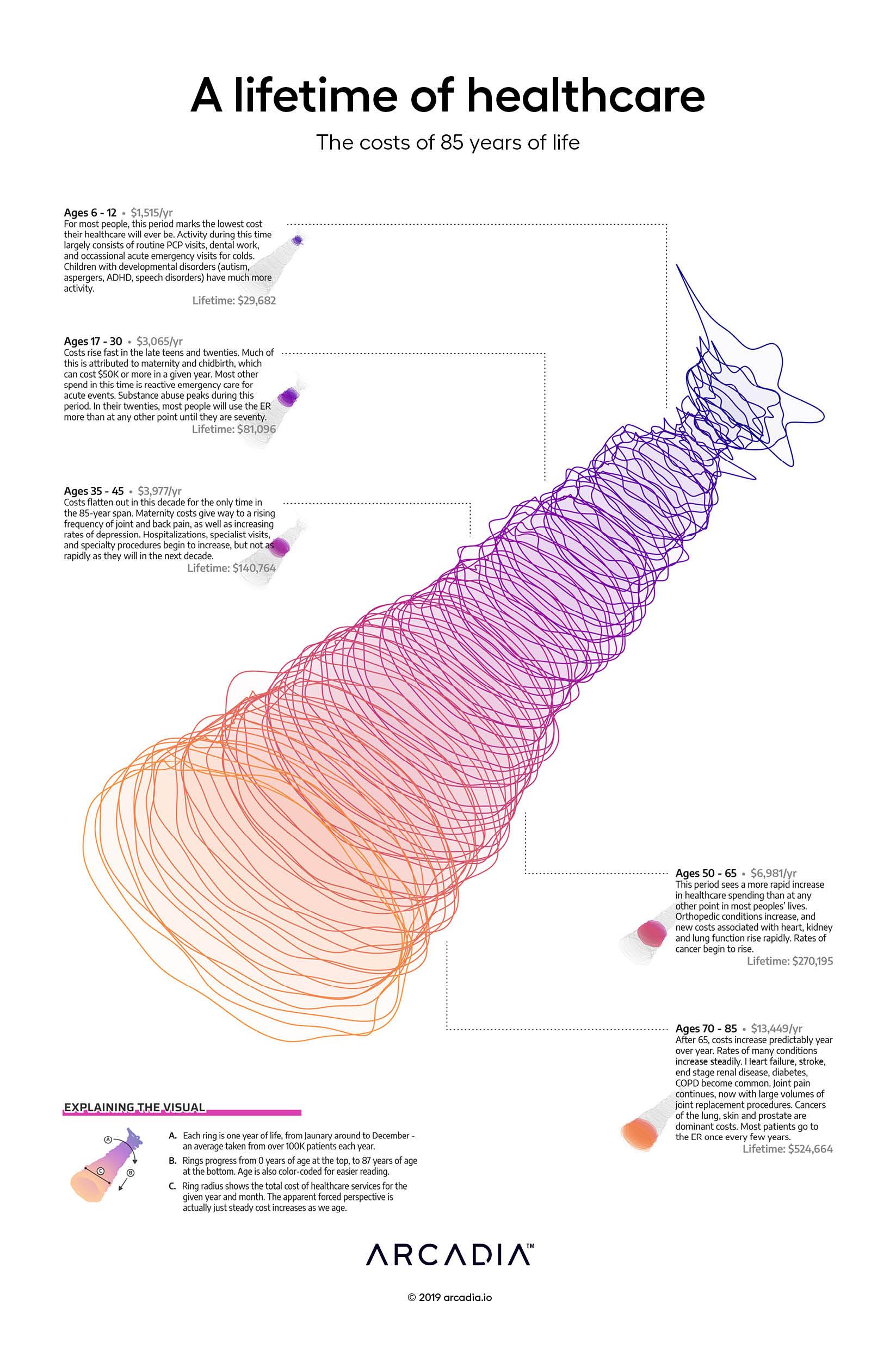
What is a lifetime of healthcare worth? Analyzing 100,000 patients at various points in their life, we track and visualize the “average” lifetime of healthcare costs, month-over-month from infancy to death.
As infants and toddlers, we incur the high costs of safely entering this world. For the healthy teenager, years go by with little more than a primary care visit or an immunization. In our twenties we tend to stop using preventive services and spend more time in the emergency room reacting to adverse events. A little older and we see those costs of maternity and childbirth come around again, but this time on the other side.
Age takes its toll. In our forty’s we are still mostly staying out of the hospital, but costs for depression and joint pain go up. The following decades see costs increase more rapidly than any other time in our lives. The aging process drives up orthopedic procedures, new incidences of cancer, and new medical needs for our hearts, lungs and kidneys.
After sixty-five, our healthcare use increases steadily. Joints are replaced, hearts and kidneys fail, and cancers become the dominant cost driver. We see the inside of a hospital more routinely and are more predictably visiting clinics for primary and specialty care.
All-in, the average lifetime of U.S. healthcare tallies a little north of $500,000 per person. But there is no average life. We pass through this world with hugely varying needs. About 80% of us will need much less than $500,000. A smaller percentage will have lifetime costs well beyond that figure. Regardless of where each of us lands on that spectrum, we hope to have a healthcare system that provides for us and lets us live our lives with dignity, to the fullest.
Details
D3.js, with Illustrator
Data sourced from Commercial, Medicare and Medicaid claims from Arcadia Benchmark Database
