Arcadia analysis of COVID-19 hospital patient data shows higher post-discharge mortality rate compared to non-COVID patients
Patients discharged for COVID-19 are 1.6 times more likely to die than a patient discharged for sepsis.
Boston, Mass., Feb. 2, 2022 — Arcadia (arcadia.io), the leading population health management and health intelligence platform, today released its analysis of data involving COVID-19 patients who were hospitalized and discharged from U.S. hospitals in 2020. The key finding is that COVID-19 patients had a high mortality rate post-discharge compared to the general population — and a mortality rate even higher than discharged patients who had a diagnosis of sepsis.
Specifically, the Arcadia analysis indicates:
- 15.1% of COVID-19 patients die in the 90-day window post discharge, including 20.6% of patients categorized as very high risk.
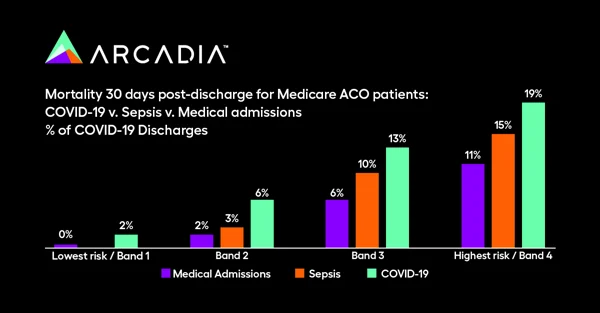
- More patients died from COVID-19 within 30 days of discharge than medical admissions or patients with sepsis across all risk bands.
- Patients discharged for COVID-19 are 2.4 times more likely to die in the 30-day window post discharge than those discharged from a medical admission. They are 1.6 times more likely to die than a patient discharged for sepsis.
Arcadia compared post-hospital outcomes for COVID-19 with post-hospital outcomes for sepsis because both categories represent life-threatening infections. The diagnostic category of sepsis usually reflects severe bacterial infections, but viral infections including COVID-19 can also present life-threatening challenges.
“This data is a sobering reminder of how ravaging COVID-19 can be to the body, both immediately and over the long term,” said Rich Parker, MD, chief medical officer at Arcadia. “It’s important for people to understand that even if you make it out of the hospital, it’s still a long journey. How many COVID-19 patients will return to functional status, to walking, talking, working, feeding themselves, versus lying in bed with a challenging quality of life? We need to make sure our high-risk patients understand how important it is to get vaccinated and boosted — the best way to avoid hospitalization.”
“Arcadia’s mission is to provide the fabric of data and insights our customers need to surface and address the needs of patient populations for improved care and outcomes,” said Jacob Hochberg, executive director of customer insights at Arcadia. “The HIPAA-compliant, NCQA- certified Arcadia Analytics platform continuously aggregates and curates up-to-date population health data assets so our customers are empowered with actionable insights. We have tremendous empathy for all the organizations we work with who are in the trenches fighting COVID, and we are constantly working to support them with data and workflow capabilities.”
Long-COVID: When symptoms last for weeks or months
Many hospitalized patients will have a long road to recovery post-discharge, but many more patients with COVID-19 will struggle with long-COVID, where symptoms of COVID-19 can persist for weeks or months with painful consequences for patients and their families.
Arcadia recently released a white paper titled, “What Drives Long-COVID? Understanding Complex Interactions with Real-World Data.” Common symptoms of long-COVID include fatigue, cough, shortness of breath, muscle and joint pain, chest pain, loss of taste and smell, difficulties in thinking or concentrating (“brain fog”), depression, anxiety, and abnormal sleep patterns. These symptoms can occur even in people who had mild symptoms of COVID-19.
As many as one in 10 people may have symptoms of COVID-19 for weeks or months after their initial infections, driving a staggering total number of long-COVID cases that continues to increase. A new study by the University of Michigan estimates that 43% of people around the world — or more than 100 million people — who have been infected with COVID-19 “have experienced lingering health concerns or are still reporting problems.”
About the study
Data for this analysis were collected from 3,836 patient records during calendar year 2020 from Arcadia Data Research (arcadia.io, Burlington, MA), a normalized, de-identified clinical and operational dataset containing more than 150 million patient records composed of data from electronic health record (EHR) systems, practice management systems, healthcare payer claims and eligibility data, care management and clinical assessment data, and other third-party sources.
To account for variation in population acuity, analysis was done across four distinct risk bands based on the CMS Hierarchical Condition Category (HCC) Risk Model:
- Risk Band 1 (6% Of Admissions): HCC risk score < 1
- Risk Band 2 (20% Of Admissions): HCC risk score between 1 and 2
- Risk Band 3 (22% Of Admissions): HCC risk score between 2 and 3
- Risk Band 4 (52% Of Admissions): HCC risk score >= 4
The cause of death was not available for use in this analysis. Patients with COVID-19 may be discharged and die for unrelated reasons.
About Arcadia
Arcadia is dedicated to happier, healthier lives for all. We transform data into powerful insights that deliver results. Through our partnerships with the nation’s leading health systems, payers, and life science companies, we are growing a community of innovation to improve care, maximize value, and confront emerging challenges. For more information, visit arcadia.io.
# # #
