Beyond the colonoscopy: BILH Performance Network's transformative approach to colorectal cancer screening
When Beth Israel Lahey Health undertook a new shared decision-making program to screen for colon cancer, they discovered the power of engagement and prevention.
According to the American Cancer Society, colorectal cancer is the third leading cause of cancer deaths in both men and women, and the second leading cause when those demographics are combined. With about 150,000 new cases of colorectal cancer in the US each year, it’s one of healthcare’s greatest challenges.
To compound this problem, screenings are growing costlier each year, particularly when they’re done in hospital outpatient departments. The math is thorny: in the calculation around priceless human lives, how can healthcare organizations reconcile the need for expensive, inconvenient testing with the necessity (and potential savings) of prevention? Innovative healthcare organizations are looking at novel ways to screen, prevent, and treat this disease.
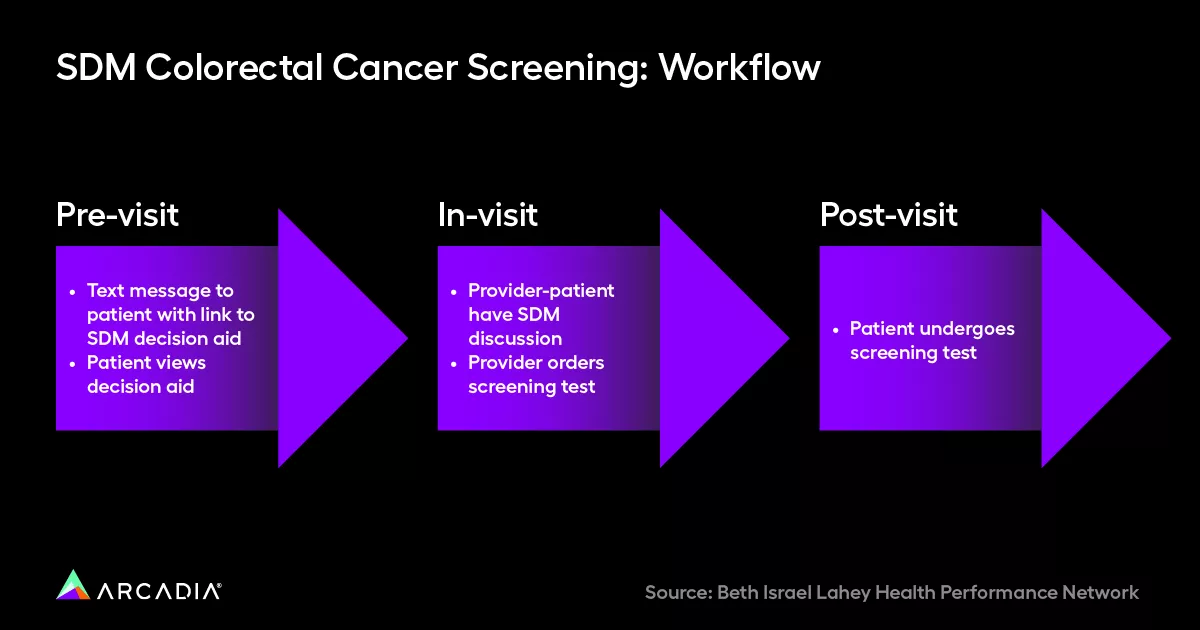
Enter Beth Israel Lahey Health Performance Network, who recognized this two-pronged issue and took a new approach in partnership with BlueCross BlueShield of Massachusetts. Through a shared decision-making model, BILH Performance Network reached out to their at-risk patients with information and options, and through a thoughtful engagement campaign, they leveraged data to ramp up screenings, lower risk, and save costs.
Here, we’ll dive their findings and explore how data, automated outreach, and innovation can help healthcare organizations navigate challenges victoriously.
Shared decisions, shared stake
To embark on this program, BILH Performance Network used data analytics to curate a pool of text message recipients between 45 and 75, specifically listed as not having been compliant for a colorectal cancer screening. They also targeted those with upcoming primary care appointments within the next 30 days, so that they could follow through on any testing.
SDM Colorectal Cancer Screening: Report identification criteria for Decision Aid Tool text messages
- Age: 45-75 and alive
- Patients listed as not being compliant for Colorectal Cancer Screening (identified by the performance within the payer contracts)
- The following risk units by Functional PCP:
- All of BIDHC practices (including the 4 BIDHC practices listed within Whittier risk unit)
- HCA (HCA: Atrium Suite, Central Suite, North Suite, South Suite) + (Residents: Atrium Suite, Central Suite, No Suite Assignment, North Suite, South Suite)
- Whittier: (BIDHC - Newburyport, BIDHC - AJH - Amesbury, BIDHC - AJH - Haverhill, BIDHC - Seabrook, North Shore Internal Medicine, Seacoast Medical Associates, Highland Primary Care Associates)
- API (7 practices will join in October 2023)
- The patient has an upcoming appointment at Primary Care office (either with PCP, MD, NP, PA, Resident)
- The upcoming appointment is within the next 30 days
- All payers included
Source: Beth Israel Lahey Health Performance Network
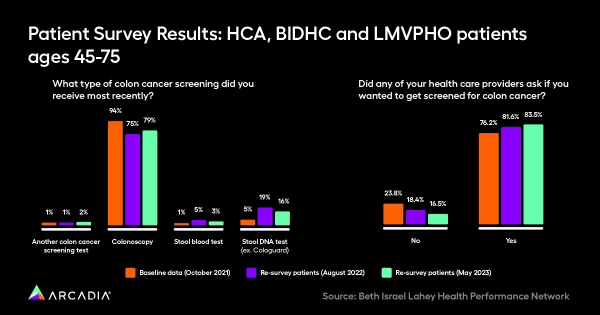
Colonoscopies (not always popular) are one way to screen for colorectal cancer, and they’re usually what doctors think of first, but a key part of this campaign’s success was offering patients choices. In this scenario, patients could explore options like Cologuard (a stool DNA test) or a stool blood test, both of which are less invasive and can be done at home, without preparation.
These options gave patients agency in their own healthcare journey, and critically, the freedom of choice was effective. A follow-up survey in May 2023 yielded a 58% completion rate, an improvement from the 37% in the baseline survey. There were eight different languages offered, from Portuguese to Italian, so that texts were tailored to their recipients. They also realized that while text messaging worked for certain demographics, certain demographics responded better to telephone calls.
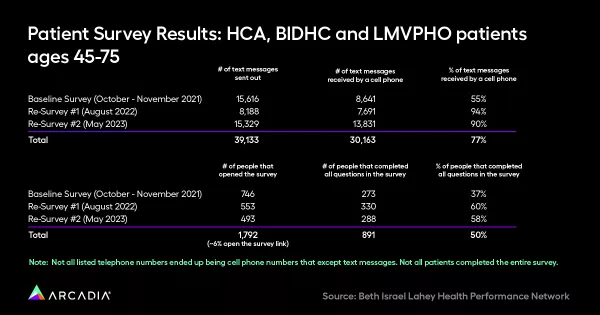
These considerations of form, content, and delivery style prioritized health equity, so that the information was accessible to many different people of many different demographics. The outreach netted nearly 1,000 total respondents, which translates to more screenings, more prevention, and potentially, more saved dollars and lives. Their texting program increased FIT DNA cancer screenings by 400%.
“There are laws that have been put in place that cover this testing in full, but people don’t know that,” Tim Carey, BILH’s Performance Network Project Manager, says. “They’re like, ‘I don’t want a Cologuard because what if it comes back positive, and I have to get a colonoscopy? I’m going to be paying an arm and a leg for that.’ That’s not true anymore.”

This level of detail may not go into a traditional campaign, but in this case, the high response rate and the increased number of screenings indicate that the information presented might matter a lot to the people receiving outreach from BILH Performance Network .
Knowledgeable patients, empowered outcomes
Before they ever provided a sample or committed to a particular type of testing, BILH Performance Network gave the patients in their study a concise but thorough decision aid tool, which explained the risks of colorectal cancer, the efficacy of screening, and the different options that were available. Then, they could indicate their level of comfort with the specific testing preparation measures on a scale of 1-10.
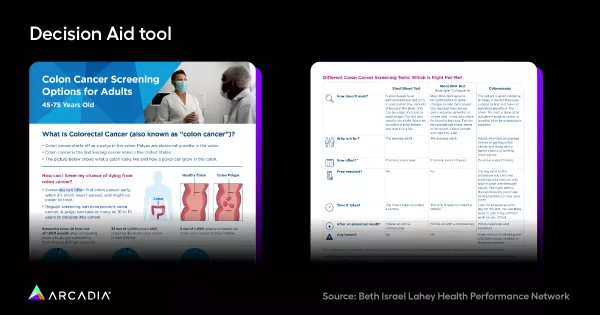
In short: as soon as patients arrived in the examination room, they had a starting point to collaborate with their provider. With the basic information conveyed, this guide could inspire additional questions or conversations that would benefit both the patient and BILH Performance Network ’s understanding of their population’s needs.
After the study was completed, BILH Performance Network found that a much higher percentage of participants had selected the Fit DNA test (28.9%) versus the general population of colorectal cancer screenings (9.1%), and knowledge like this could help BILH Performance Network tailor future programming. If patients are more likely to complete this test (versus, say, a colonoscopy), it could become the first option a provider brings up in screening conversations going forward. It might also be more effective: one study found that a FIT test had better sensitivity than an FOBT, which was much more popular amongst people who hadn’t been part of BILH Performance Network 's SDM group.
Additional knowledge shaped participants’ decisions, and this in itself is valuable for tailoring future public health and prevention efforts.
Why colon cancer prevention matters in value-based care
Keeping patients healthy is every hospital’s goal, but in value-based care, diseases like colon cancer present an opportunity to offer preventive care that saves both lives and resources. Thinking outside the traditional in-clinic colonoscopy allowed BILH Performance Network to meet patients where they were, offering convenient options that could still detect major illness.
All Risk Payers: Number of Colorectal Screenings Completed in CY2022 – YTD 2023
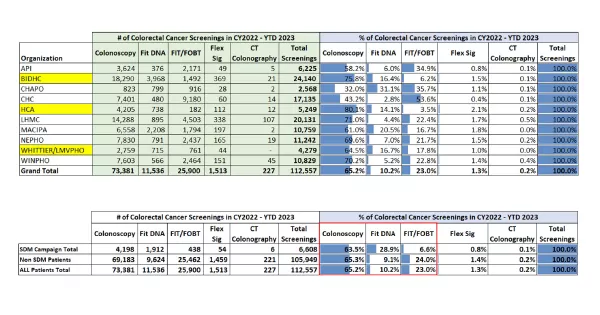
A long, protracted illness comes with incalculable costs to the patient, and to the hospital, they can be a monetary figure that balloons with every intervention. Here, the idea is that a screening — whether its in-clinic or at home — is worth the investment in future health and prevention.
Ultimately, this proactive outreach with screening and test kits may save lives and improve costs and outcomes. If colorectal cancers are detectable and preventable, it’s healthcare’s mission to deliver those screenings in a way that works for both populations and the providers who serve them.
Drive outcomes, prevent disease, repeat
In total, BILH Performance Network conducted 135,521 screenings in the 2022 calendar year, spanning patients insured by 12 different payers. For such a vast number of lives, they were able to gather an equally massive data set. As they work to keep patients in Massachusetts and New Hampshire healthy, they can draw on this knowledge into the future, continuously improving their delivery of testing and care.
Ready to drive a successful prevention campaign of your own? Learn more about data-powered outreach and engagement and leverage Arcadia’s platform for the data you need to drive continuous improvement.
