A strong single-provider relationship could reduce avoidable emergency department visits by 22%
A strong patient-provider relationship can radically improve patient outcomes and reduce unnecessary costs. Discover how you can strengthen the provider-patient bond and improve overall performance.
If healthcare organizations search for problems — unnecessary emergency department (ED) visits, high mortality rates, low HCC risk closure, and low quality measurements — they might be able to trace them back to a single source: weak patient-provider relationships. In recent data, Arcadia found that a strong single-provider relationship reduced avoidable ED visits by 22% and lowered risk-adjusted PMPM costs by 15.3%.
Whether you’re measuring in lives, dollars, or data points, patient-provider relationships exert a major influence on healthcare. Here, learn how your organization can strengthen these bonds and measure current performance, so you can provide better care and improve outcomes.
Primary care providers have stronger connections with their patients in top-performing Medicare ACOs
When it comes to provider performance, data offers proof that loyal patient-provider relationships bend the cost curve. Arcadia’s analysis shows that the top quartile of Medicare ACOs has a 29% higher rate of primary care physician (PCP) visits compared to lower performers.
This could be because primary care physicians are so often the “bridge” between a patient and the rest of their care team. If a patient needs routine lab work or is late for their annual physical, their PCP is likely the first to discover this gap in care, and the most likely team member to facilitate a follow-up or referral.
Additionally, consider the behavior of a patient without that primary resource. Maybe their conditions worsen until they’re acute. Maybe they don’t receive preventive care at all. In any circumstance, a PCP with a strong connection to their patient is a consistent touchpoint for gathering data, and a way to reach that patient for consistent treatment and care.
How the Provider Strength Score measures the impact of patient-provider relationships
A data analytics platform with utilization-based metrics, like Arcadia’s Provider Strength Score, can look specifically at primary care, classifying patients as a single-provider relationship if they received at least 75% of their primary care services from the same provider. It works by:
- Quantifying the relationship between a patient and the provider they see for primary care services: This could be one provider or multiple providers.
- Relying on utilization-based data, including providers that may or may not be attributed as the patient’s PCP: It looks back at the most recent three years of utilization data and applies more weight to more recent utilization events.
This information is available for both data analysts and clinical and operational care teams so that a healthcare organization can understand the impacts of these relationships on everything from business to clinical outcomes.
4 ways strong patient-provider relationships lower costs in healthcare
Recent data shows precisely how strong or weak provider-patient relationships impact a healthcare system’s outcomes and cost curve. Specifically, the greatest impact happens in four areas:
1. Reduce ED utilization
Across different HCC risk scores, from low to high, one correlation proves clear: patients who see a single provider consistently for their primary care services lower avoidable ED utilization by 13% to 30%.
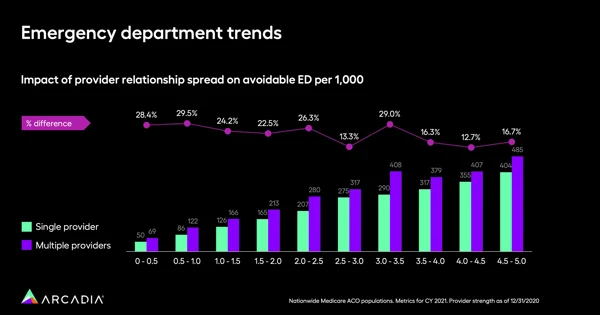
2. Lower HCC risk scores
More broadly, a strong PCP relationship reduces risk. For HCC risk bands from 0 to 1.0, there was a marginal additional decrease in risk for those with a strong PCP relationship, but as the risk bands move further up, that difference grows. For patients with HCC risk scores of 1.0 and above, a consistent primary care resource could mean closing 7.3% to 8.7% more risk. This translates into savings on chronic disease and preventable illnesses, and better performance in risk-based contracts benefits healthcare systems’ bottom lines.
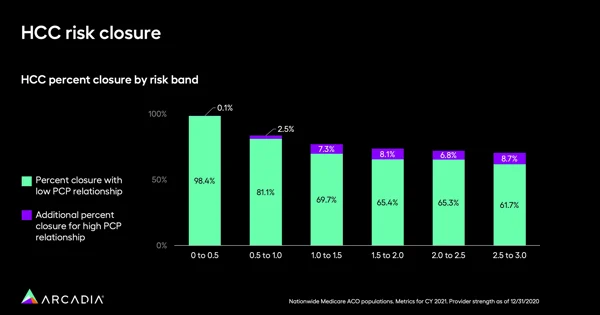
3. Improve quality measures
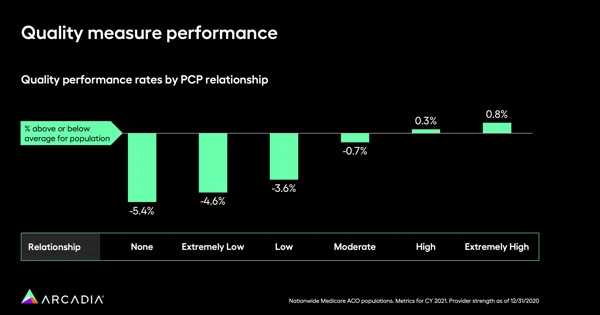
Quality measures also have a strong correlation between those with consistent PCP interactions and patients without a PCP or with a weak relationship. Patients with none whatsoever average 5.4% below average quality scores. Across the board, moderate to extremely weak relationships see substandard quality measures, while high or extremely high rates of loyalty to a PCP boost that score above average by 0.3% to 0.8%.
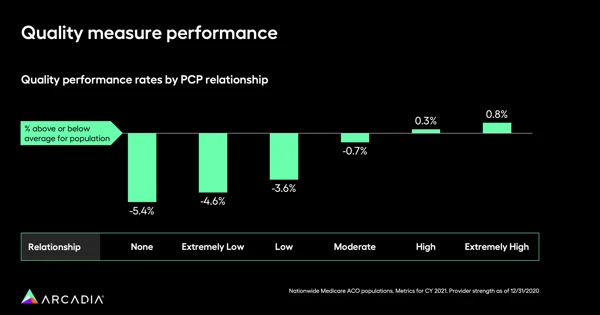
4. Reduce mortality rates and skilled nursing facility (SNF) utilization
Data also shows that patients with a weak or non-existent PCP relationship have a higher mortality rate. Patients in the 2.5 to 3.0 HCC risk category with a weak Provider Strength Score are 52% more likely to die than those with the same level of risk and a strong single-provider relationship. The same correlation applies to SNF utilization, where patients with a low PCP relationship spent more days in these care facilities.
3 areas health systems can put the Provider Strength Score to work in service of better outcomes
Once you’ve identified providers whose patient relationships are weak, it’s time to equip them with the tools to improve. This can be a sensitive conversation, but it’s a critical component of strengthening those bonds. This could involve training providers in better communication and engagement strategies, and enrolling patients in systems that support continuity of care, such as care management.
In every provider’s mind, they provide the best, highest-quality care for their patients, and that’s absolutely true. But are you capturing all that work you’re doing, all that amazing quality of care that you’re providing for your patients? We want to give you credit for it. It’s always a very humbling conversation, but as time goes by, it’s getting a little bit easier.
ED utilization
To reduce unnecessary ED utilization, office staff can use a data analytics platform to run reports targeting frequent ED patients. From there, they can educate this group of patients on after-hours protocol and resources to suggest alternatives to an emergency room visit, from telehealth services to lists of urgent vs. non-urgent symptoms. This is also a great chance to encourage support staff to assess their internal office hours protocol and patient communication.
If a clinic isn’t providing materials in Spanish, for example, but noticing a high proportion of Spanish-speaking patients visiting the ED, providing dual-language messaging could be an easy solution that lowers unnecessary usage. Providers can speak to patients that are frequently visiting the ED in an attempt to mitigate those symptoms with more consistent treatment, or screen for possible causes.
High-risk cohorts
Healthcare administrators can help providers identify high-risk patients and then encourage them to proactively address these risk gaps. Providers with a large volume of high-risk patients might be good candidates for education on proper documentation and coding.
A high-risk patient report allows office support staff to see which patients should be called to get them on the schedule.
Panel management
In Arcadia, providers can use the Vista Panel Management dashboard for transparency into their patient populations. A bird’s-eye view of population health using healthcare dashboards provides insight into frequent issues or diagnoses that they’ve frequently failed to address.
Office staff can use Arcadia’s Patient Registry report to identify more patients who would benefit from a scheduling call, keeping them in the system, and reducing their chance of forgoing care.
Lower risk-adjusted PMPM costs by 15.3% with stronger patient-provider relationships
The numbers say it all: patient-provider relationships are a matter of life vs. death, dollars vs. cents, poor outcomes vs. excellent ones. A data analytics platform with utilization-based metrics gives you the tools you need to improve single-provider relationships in your patient populations.
