Predictive analytics in healthcare: A comprehensive guide
In the unpredictable and often emergent environment of the healthcare industry, teams across the care continuum need proactive approaches to stay ahead. Predictive analytics is a key component of success across teams, enhancing patient outcomes, financial performance, and operational efficiency.
In this article, we’ll provide a comprehensive guide to predictive analytics, including:
FAQs about predictive analytics in healthcare
What is predictive analytics in healthcare?
Predictive analytics in healthcare is a type of analytics that evaluates current and historical data to predict future events. The process involves applying statistical modeling, data mining, artificial intelligence (AI), and machine learning to health data to enable accurate forecasting.
Predictive analytics applies to many types of healthcare data, including:
- Structured data, like demographic data and laboratory test results
- Unstructured data, such as clinical notes and imaging
It also leverages big data to provide insights into patient care, resource management, and health outcomes.
What is predictive modeling in healthcare?
Predictive modeling is the process of running mathematical algorithms on data to predict what’s most likely to happen in the future.
Although the terms are often used interchangeably, predictive modeling is considered a subset of predictive analytics. Predictive modeling describes the process of building a statistical model, while predictive analytics refers to the entire process of using data to make predictions.
How does predictive analytics work?
The journey of predictive analytics in healthcare involves four stages: data collection, preprocessing, modeling, and interpretation of results. Click through each stage below to explore what it entails:
Predictive Analytics in Healthcare
Click on each stage to explore how data transforms into actionable healthcare insights
Data Collection
Preprocessing
Modeling
Interpretation
What are the benefits of predictive analytics in healthcare?
By leveraging predictive analytics in healthcare, organizations can experience the following benefits:
- Patient stratification: Predictive analytics enables early diagnosis and preventive care by identifying health risks before they escalate. Proactive insights are especially indispensable for chronic condition management, as heart disease and cancer are the leading causes of death and disability in the U.S.
- Automated patient messaging: Predictive analytics allows providers to send messages tailored to specific audiences. Thoughtful, dynamic content can promote preventive care and engage patients, so they’re more likely to continuously pursue better health.
- Registry and care gap lists: Predictive analytics helps identify polychronic patients (those with three or more chronic diseases) and quickly surface insights so healthcare organizations can offer additional care.
- Care management: To pinpoint high-need patients, choose the right interventions, and coordinate care accordingly, care managers need software with predictive capabilities. Additionally, predictive models enable care managers to orchestrate post-acute flows by monitoring patients’ progress and intervening proactively if needed.
- Point-of-care decision support: For clinical teams, predictive analytics augments diagnostics with advanced machine-learning algorithms and can prove invaluable in managing emergencies through real-time data analysis.
- Clinical documentation improvement: Predictive analytics helps measure risk and anticipate quality. With analytics tools, care teams can zero in on the information that matters most to manage a patient’s risk.
- Medical economics research and contract design: Predictive analytics serves as a compass for long-term strategic planning for analysts and actuaries. These professionals can better assess financial risks and sustainability, ensuring a balanced approach to healthcare financing.
- Data visualization and dashboard design: Analysts and actuaries can also leverage predictive analytics to distill their valuable insights into shareable images and dashboards so that other stakeholders can better understand performance and goals.
- Research and model design: Predictive analytics bolsters the development of breakthrough treatments and drugs. Data mining and pattern recognition, which are essential for drug development and clinical trials, heavily rely on predictive analytics.
How does predictive analytics benefit different healthcare teams?
Predictive analytics offers benefits to many teams across the care continuum. For example, a provider may reference a list of helpful questions for the at-risk pre-diabetic patient sitting in front of them. Meanwhile, a data scientist may build a model that transforms care delivery in a hospital’s oncology unit.
See how the benefits described above impact different health teams:
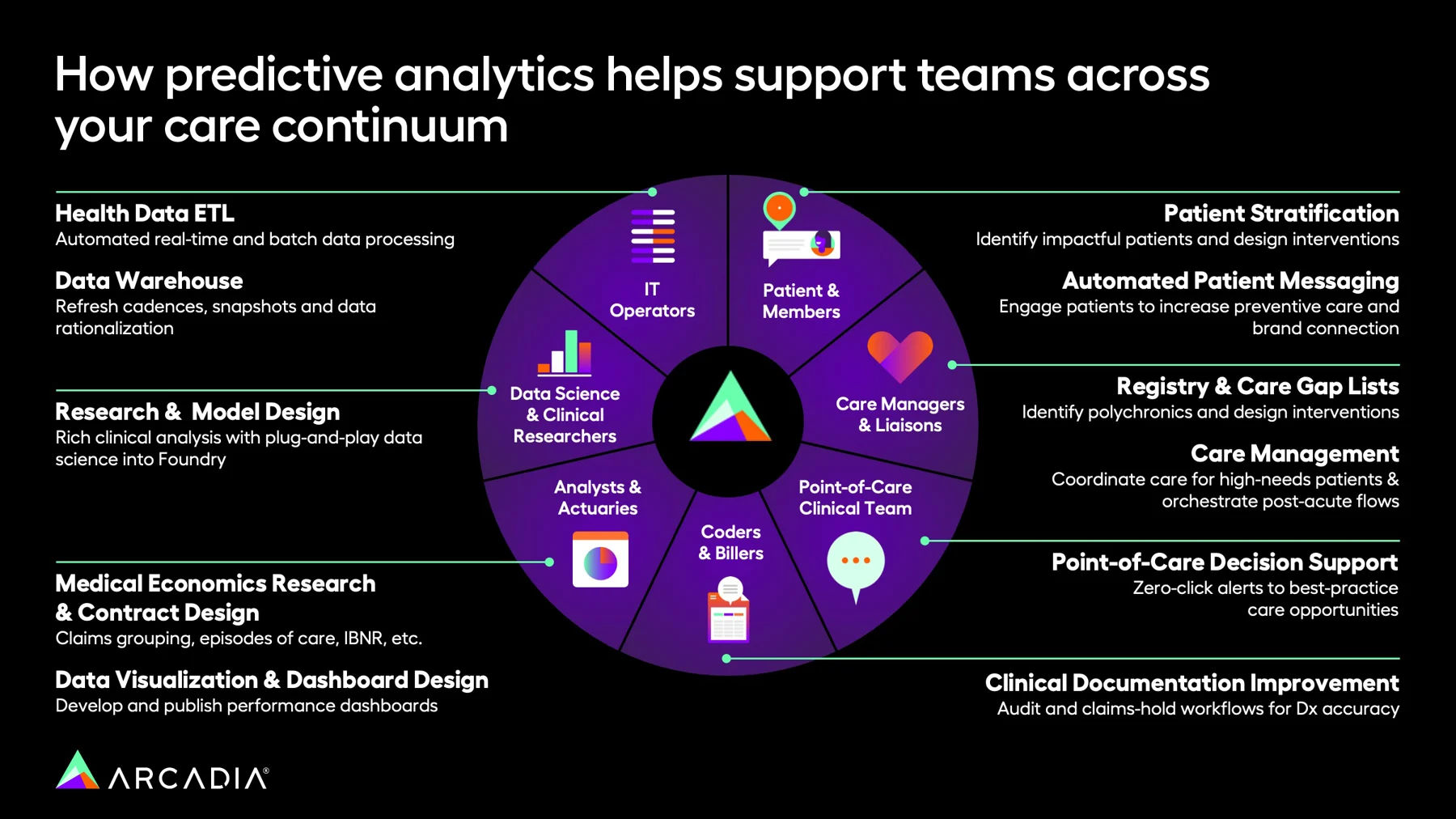
- Patients and members: Care managers and clinical teams can use predictive models to create treatment plans tailored to each patient's profile. Additionally, this form of analytics powers early reminders and helps providers encourage preventive care (e.g., screenings or vaccinations).
- Care managers and liaisons: Care managers may also use predictive analytics to allocate time and resources where needed most. This enhances patient engagement and satisfaction by ensuring care is timely and efficient. It also allows care managers to better target interventions, significantly improving outcomes.
- Point-of-care clinical teams: Clinicians face immense pressure to choose the right course of action or diagnosis amid a sea of options. Predictive analytics eases some of this burden by providing point-of-care decision support that helps clinical teams arrive at the best solution more quickly.
- Coders and billers: Forecasting future events can help coders and billers refine processes to recoup wasted time and create efficient workflows. For this team, predictive analytics also plays a crucial role in fraud detection and in assessing billing error risk.
- Analysts and actuaries: Predictive insights enable analysts and actuaries to translate data into actionable information that drives informed decision-making.
- Data science and clinical researchers: Predictive analytics can be the key to new discoveries in clinical research. It enables more thoughtful studies and sharper insights around central questions.
- IT operators: By properly structuring and organizing an organization’s data, IT operators expand other users’ predictive analytics capabilities with reliable, vetted information.
How is predictive analytics used in healthcare?
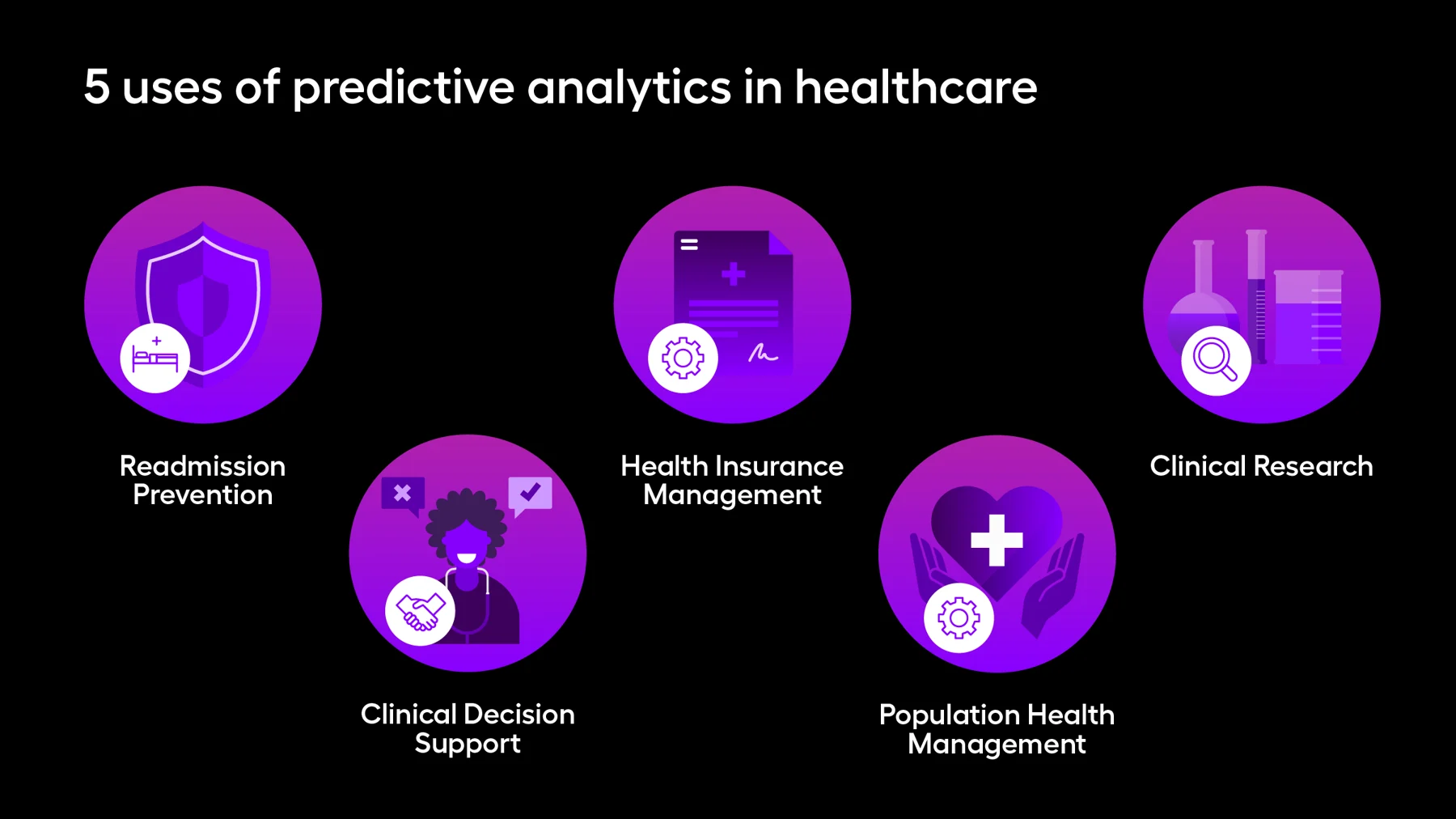
1. Readmission prevention
With nearly one-in-five adult patients experiencing hospital readmission, healthcare providers must proactively address patients’ follow-up needs with personalized discharge protocols. Using healthcare predictive analytics, providers can identify patients at risk of readmission and allocate resources to prevent this turnaround.
In addition to benefiting the patient, preventing hospital readmissions also reduces unnecessary costs across the healthcare sector, which are currently estimated at $52.4 billion per year in total.
2. Clinical decision support
Predictive analytics enables clinicians to anticipate patient outcomes, optimize treatment plans, and improve overall care quality. With predictive analytics, clinicians can:
- Diagnose conditions early: Identify early signs of diseases that may be difficult to detect in the initial stages
- Select treatments: Forecast a patient’s response to specific treatments to reduce the need for trial-and-error approaches
- Monitor critical conditions: Analyze real-time patient data to spot early warning signs and improve patient outcomes
When clinicians are equipped with the full context of a patient’s needs, they can make informed decisions with confidence in positive patient outcomes.
3. Health insurance management
With regard to health plans, predictive analytics provides insights into:
- Care utilization: Providers can proactively meet care needs and mitigate unnecessary costs through predictive analytics. This allows them to accurately forecast a patient’s healthcare utilization, such as hospital admissions or surgeries, based on historical data and clinical variables.
- Predicted costs: A patient’s expected healthcare costs can be forecast by understanding their past utilization and treatment needs. By calculating the likely cost of care, health plans can set appropriate premiums and manage risk proactively to help minimize unnecessary spending.
- Fraud prevention: Payers can analyze claims data to identify fraudulent behavior patterns, detect them early, and prevent insurance abuse. This significantly impacts healthcare costs, as financial losses from healthcare fraud account for 3% to 10% of healthcare spending, or $300 billion.
Calculating the accurate cost of insurance empowers patients to receive the care they need without financial hindrances.
4. Population health management
Providers can take patient data beyond individual care to identify cohorts with shared medical characteristics and prevent population-wide health risks. For example, providers may detect disease outbreaks early by using predictive analytics to identify groups with potential exposure. As a result, providers can improve population health management efforts by developing treatment plans in a timely manner.
5. Clinical research
About 90% of drugs fail clinical trials. However, research suggests that artificial intelligence can help alleviate the issues behind these failures. Using predictive analytics, AI can:
- Identify eligible patients for drug trials
- Enroll those who are likely to participate
- Determine appropriate sample sizes
- Reduce inconsistencies in protocol
- Allocate clinical funding more effectively
By addressing these issues, the technology behind predictive analytics enables researchers to conduct trials more efficiently, increasing the likelihood of reaching groundbreaking results.
Challenges and ethical considerations for implementing predictive analytics in healthcare
Despite its many benefits, predictive analytics in healthcare has risks and challenges. Some top concerns include:
- Data security and privacy: Given the sensitive nature of health information, healthcare data is a huge target for cybersecurity issues. To maintain patient trust, comply with HIPAA regulations, and protect human privacy, providers must employ strict data security measures.
- Accuracy and reliability: Predictive models are under constant scrutiny to avoid potential misdiagnoses, biases, or treatment errors. This leads to a lack of trust in the model.
- Provider acceptance: Providers must balance the need for enhanced patient care through data collection with the time and effort required to leverage analytics. From training on new technologies to implementing new workflows, the process may involve significant changes for providers.
This doesn’t necessarily spell doom for predictive analytics in healthcare. By enforcing data access controls and obtaining consent before sharing data, providers can benefit from predictive analytics while still protecting patient privacy. Still, it does mean that users need to approach any technology with a clear sense of when it’s appropriate, how to avoid missteps, and how to read results with a critical eye.
Ethical considerations, such as addressing healthcare disparities and mitigating bias in data and algorithms, also need ongoing attention. For example, implicit biases can find their way into predictive analysis algorithms, leading to unfair outcomes. You’ll need to critically examine algorithmic outputs to eliminate any biases.
Umpqua Health: An example of predictive analytics in healthcare
Umpqua Health is a community care organization serving 35,000 Oregon Health Plan Medicaid members in Douglas County. When wildfires consumed more than 100,000 acres in the state during the 2020 and 2021 fire seasons, Umpqua responded by distributing air purifiers to members affected by the poor air quality from wildfire smoke.
However, people with respiratory conditions are at greater risk of harm due to the smoke from these fires. In anticipation of the next wildfire season, Umpqua wanted to proactively distribute air purifiers to those who needed them.
Using Arcadia’s platform to analyze SDoH data, past events, and claims data, Umpqua predicted individuals’ future risk for respiratory complications. Hear how these insights surprised the organization and informed their strategies in the following clip featuring Dr. Robin Traver, Umpqua Health’s Senior Director of Medical Management:
Takeaways for predictive analytics in healthcare
Predictive analytics impacts every facet of healthcare and opens up exciting possibilities, from earlier interventions to a more customized, thoughtful, and engaging patient experience. As a powerful tool for enhancing healthcare delivery, it offers insights that are instrumental in driving efficiency, accuracy, and improved patient outcomes.
The future trajectory of predictive analytics in healthcare is both promising and challenging. Emerging technologies like AI significantly augment predictive analytics capabilities, and healthcare providers must embrace this technology to stay at the forefront of healthcare innovation.
Success in predictive analytics requires the right foundation, and a sophisticated architecture (like a lakehouse) is the first step in leveraging this technology. The integration of these technologies into healthcare workflows is vital for realizing their full potential and improving patient outcomes and operational efficiencies.
With the right mix of thoughtfulness and innovation, technology advocates and healthcare pioneers can collaborate toward a more predictive and proactive healthcare system.
