Healthcare data warehouse benefits, features, and use cases
The healthcare industry generates an unprecedented amount of data each year — approximately one-third of the world’s total data volume. This data holds the power to drive informed decision-making, yet a staggering 97% of it goes unused.
As technology increasingly addresses the challenges of harnessing this data, the healthcare data warehouse emerges as a popular tool for aggregating and analyzing data. This article provides a detailed overview of this software, including:
FAQs about healthcare data warehouses
What is a healthcare data warehouse?
A healthcare data warehouse (HDW) is an organized central repository for aggregated healthcare information. The tool retrieves data from multiple sources, such as:
- Electronic health records (EHRs)
- Electronic medical records (EMRs)
- Enterprise resource planning systems (ERPs)
- Radiology results
- Lab databases
- Wearable devices
- Population-wide data
How does a healthcare data warehouse fit into a data platform?
A healthcare data warehouse is only one key component of an integrated healthcare data platform, which includes:
These platform processes compose a data platform pipeline that collects and transforms raw data into usable analytics for your organization’s decision-making and integrates actionable intelligence into workflows.
HDWs are the fourth component of a healthcare data platform, and the prior components (the connectivity layer, data lake, and analytics enrichment processes) determine the volume and type of data stored in an HDW.
It’s worth distinguishing between a data lake and a data warehouse, as you want these two components to remain separate. A data lake represents raw data in its unusable form, while an HDW is an organized storage location of usable data.
What are the benefits of healthcare data warehousing?
By leveraging a data warehouse, healthcare teams can experience benefits like:
- Efficient reporting: HDWs can help your team quickly create precise analytics reports to get a bird’s-eye view of your healthcare cost and quality performance. For example, your team can use dashboard reporting to efficiently compare high-cost members across cohorts (admission, drug, condition, etc.), total members, and total cost.
- Improved clinical decision-making: Discover the right insights at the right time by integrating a unified HDW into existing workflows. Rather than using siloed databases and systems, an HDW can connect all your information and tools across the enterprise.
- Optimized insurance claims and payments: Your healthcare organization can review and efficiently process large amounts of claims data, access and analyze information within those claims, and use those insights to improve performance and outcomes.
- Elevated strategic planning: Take a comprehensive approach to resource planning with accessible data tools. Use data gathered from disparate sources to identify and avoid future challenges.
- Enhanced patient satisfaction and outcomes: For patients, an accessible HDW means they can receive timely, accurate treatment informed by advanced analytical models and experience measurable progress.
- Personalized value-based care: Collaborate with other clinicians using a uniform HDW to generate deeper insights and enhance treatment plans for patients while avoiding unnecessary costs.
What are the key features to look for in a healthcare data warehouse?
HDWs are inherently sensitive and require proper handling to meet security measures while integrating successfully with various data sources. Additionally, each HDW is tailored to a specific organization’s needs, so the key features will differ depending on the HDW’s proposed end-use.
However, there are common aspects worth paying attention to, regardless of your team’s custom HDW model. A fully functioning HDW will include:
- Data integration: HDWs field data from EHRs, ERP software, HR management systems, claims management systems, and large public health databases. This data integration includes big data and streaming data in addition to advanced medical data loading and querying. Make sure your HDW is equipped to standardize data from both internal and external sources.
- Data quality: Successful HDWs include quality controls for data accuracy, completeness, and consistency. Built-in processes like data cleaning and validation help to promote standardization across data points.
- Scalability: Your organization could start with a relatively simple HDW configuration, but with increased use, you will likely need to rely on a scalable solution. A robust HDW built with future data volume in mind will help you make sense of larger data loads.
- Security and privacy: Correctly built HDWs have encryption and access controls to protect patient data. Raw-level permissions by account or patient ownership keep HDWs aligned with US Federation laws, such as HIPAA.
- Interoperability: Efficient HDWs make fragmented workflows a thing of the past by bringing operational care teams together to collaborate for whole-person care. Your HDW should be set up with care coordination ease in mind.
If you decide to go with a single or multi-data platform provider, verify that they offer the above features. Or, if you decide to advise an in-house team, build your data platform with these outlined aspects. That way, you can maximize your analytical horsepower and generate the highest ROI for your time and efforts.
Challenges in healthcare data warehousing
Data silos and interoperability issues
The power of health data lies in the capacity to analyze and extract insights from it. However, health data is often fragmented due to the complexity of the integration process, which hinders data exchange between teams across the care continuum.
A significant contributor to this issue is the lack of standardization across data sources. Health information is, by nature, heterogeneous because of the various formats used in EHRs, imaging platforms, and other databases. These inconsistencies force healthcare data warehouses to aggregate incongruous records, making it difficult to access a holistic view of patient information needed to deliver high-value, low-cost care that makes healthcare sustainable.
Keeping your HDW unstructured and unusable will result in disorganization and breakability issues further down the data platform pipeline. Applications and integrations, therefore, will pull from potentially faulty data. That’s why many healthcare organizations partner with vendors like Arcadia to bridge the gap between an overflowing data lake and an effectively structured HDW within a holistic data platform framework.
Assurance of data quality and integrity
Just as damaging as fragmented information, erroneous and incomplete data can lead to misguided decision making, duplicative efforts, inefficient use of resources, and missed opportunities to impact a patient’s outcome
Key challenges include:
Missing or incomplete data: Failing to collect or store critical information, such as medication history and social determinants of health (SDoH) data, can impair medical decisions.
Duplicate data: Redundancies resulting from disparate systems can distort population health metrics.
Invalid data: Typos, outdated codes, and inconsistent terminology across systems risk clinical and analytical errors.
Healthcare data warehouses must come fully equipped with quality controls like data cleaning and validation processes. Otherwise, healthcare organizations risk basing their decision-making on unreliable data, ultimately impacting the bottom line.
Compliance and security concerns
Healthcare data warehouses store sensitive patient information, making them prime targets for cyberattacks and data breaches. In fact, the healthcare industry is one of the most frequently targeted sectors by cybercriminals.
Health organizations need a framework to properly handle data, ensuring its accuracy, accessibility, and security. A strong data governance framework includes:
- Data quality: High-quality data means fewer errors in patient records, more accurate risk adjustment, and better clinical and financial outcomes.
- Data management: Effective practices should standardize data collection, storage, retrieval, and usage to streamline operations and improve patient care.
- Data policies: Guidelines governing data access and handling protect patient privacy and ensure compliance with regulations such as HIPAA.
Protecting patient data requires a multifaceted approach that combines secure technology with organizational policies. As mentioned previously, the right healthcare data warehouse will offer encryption and access controls to protect patient data.
Common healthcare data warehouse models
There are two common healthcare data warehouse models that different solutions use: The enterprise data model and the independent data mart model. Let’s take a closer look at each of them.
Enterprise data model

This model represents a top-down approach that most analytics vendors promote, as organizations typically use it when they need additional analytic capacity.
The goal of this model is to create the perfect database from the start by determining everything your organization would like to analyze in advance to improve specified outcomes. For instance, you might decide to prioritize safety and cost-effectiveness and structure your HDW with that end goal in mind.
Although a common model, the enterprise data model promotes an early-binding approach that can delay time-to-value. This means that once the data is bound, making changes is difficult and time-consuming. Therefore, within the ever-changing landscape of healthcare, enterprise models can pose significant challenges when new analyses are needed.
Independent data mart model
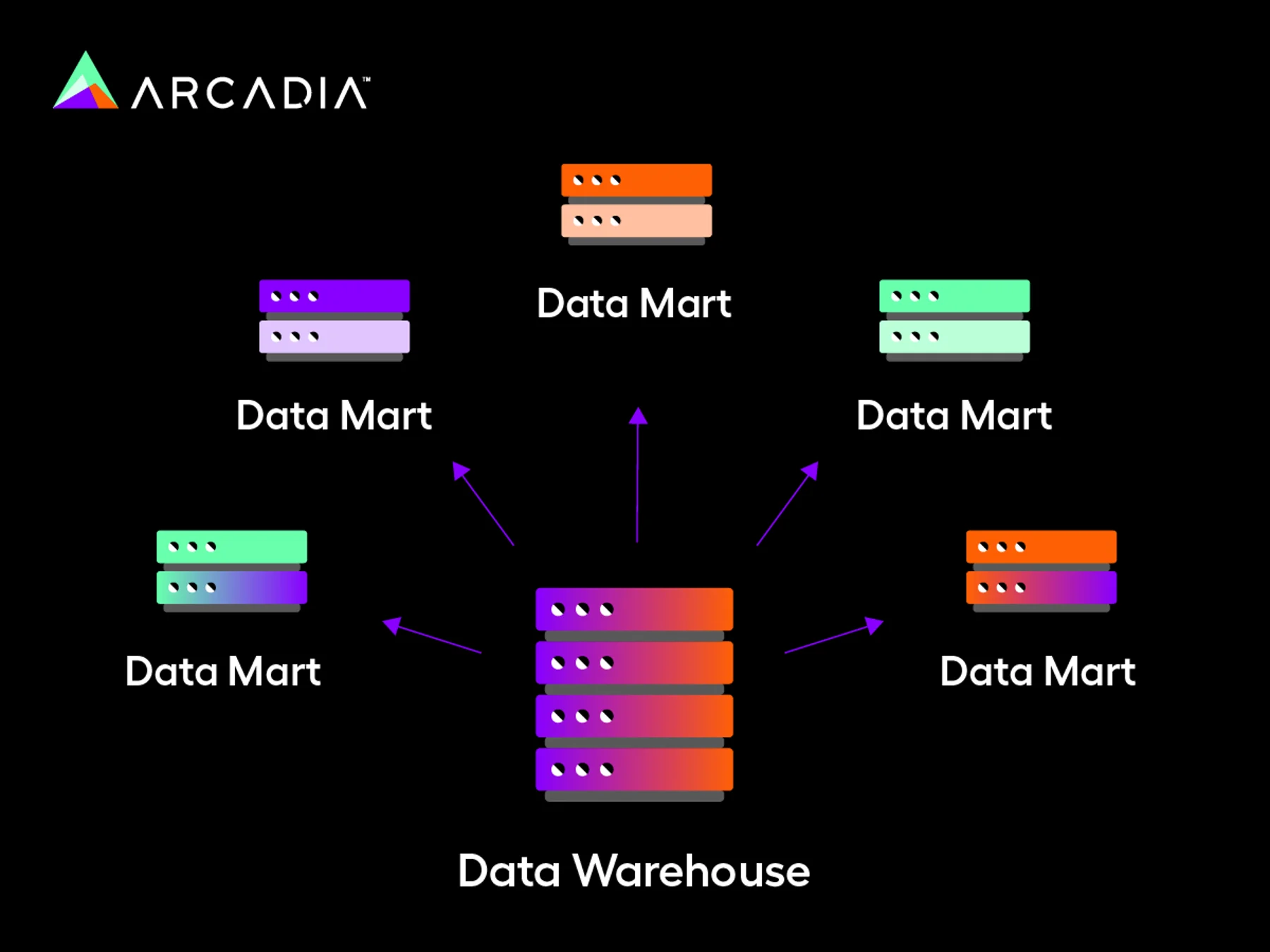
This model advocates for a bottom-up approach and is commonly used for ad hoc analysis since it can build individual data marts for individual departments. For instance, if you need a specific report on patient safety or medical cost containment, your department can build it quickly using this model.
Independent data mart models are inherently smaller and more focused than enterprise data models. They can help your team implement and measure needed metrics much more quickly than enterprise data models. However, independent data marts can also overwhelm systems quite easily and cause data redundancy issues down the line.
Healthcare data warehouse use cases
Treating chronic conditions
Accurate data and timely analytics are critical for serving populations facing chronic conditions.
For example, diabetes affects 40.1 million Americans — a staggering 12% of the population. Measuring and monitoring this disease is especially important because, if left untreated, it can be a catalyst for several other negative health outcomes, such as kidney disease, blindness, stroke, or even death. Accurately and specifically documenting patient conditions is critical to deliver whole-person care.
By incorporating a healthcare data warehouse into chronic care management, health teams can:
- Leverage SDoH (social determinants of health) data like risk factors, trends, and pattern identification to improve outcomes and performance.
- Support disease management initiatives, such as glucose level checks and medication adherence.
- Provide insights to prevent comorbidities and worsening symptoms with appropriate care.
Diabetes is common and involves highly personalized treatment plans to effectively manage. With a robust HDW, your team can successfully manage diabetic and chronic condition patient cohorts within value-based care programs.
Improving end-of-life care
Adequate hospice care gives patients and their families the dignity they deserve during a patient’s final moments. Tracking and visualizing Medicare patients who have passed away can help organizations understand how to improve end-of-life care.
By tracking the cost per patient during their final thirty days, analysts found that:
Patients with adequate hospice care saw regularly increasing costs to the day of their death.
Patients with no hospice care saw costs spiral out of control.
Patients with inadequate hospice care saw a sharp increase in costs that stabilized in their final days.
The ramifications of this data suggest a relationship between adequate hospice care and a more comfortable, higher-quality end-of-life experience.
Final thoughts on healthcare data warehouses
A robust data infrastructure is no longer the future of healthcare — it’s the present. Every data point represents an individual, and your organization’s ability to collect, streamline, and analyze each point directly impacts your ability to deliver better care, increased revenue, and reduced costs.
Partnering with an experienced data vendor like Arcadia can help you succeed, no matter your journey in fee-for-service, value-based care, or beyond.
